What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
Medications to Avoid After Gastric Bypass
Gastric bypass has become an increasingly common option for patients seeking permanent weight loss. Because many patients who are gastric bypass candidates often have other chronic health conditions that require maintenance medication, it is important to know which medications are safe to take after gastric bypass and which are not. After bypass, the anatomy of the stomach and intestines is changed, affecting how medications function and how these medications affect the gastrointestinal tract.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
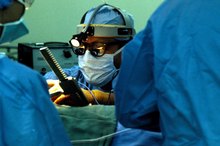
Gastric Bypass Surgery
A type of bariatric weight loss surgery, gastric bypass involves greatly reducing the capacity of the stomach using staples to create a small pouch at the upper part of the stomach 2. The small intestine is then connected to the pouch. Because the stomach pouch has a greatly reduced volume, patients can eat less and lose weight. The absorption of some medications is also changed because of this change in anatomy.
- A type of bariatric weight loss surgery, gastric bypass involves greatly reducing the capacity of the stomach using staples to create a small pouch at the upper part of the stomach 2.
- Because the stomach pouch has a greatly reduced volume, patients can eat less and lose weight.
Extended Release Medications
Differences Between Strattera & Concerta
Learn More
Extended release medications are not a viable option because the anatomy of the stomach is greatly altered in gastric bypass. Extended release medications work by dissolving in the stomach slowly and are then released into the bloodstream at a slower, more even rate. Because gastric acids and enzymes are reduced or altered after gastric bypass, this mechanism does not work as it normally would. Extended release medications also cannot be crushed or chewed.
- Extended release medications are not a viable option because the anatomy of the stomach is greatly altered in gastric bypass.
NSAIDS
Non-steroidal anti-inflammatory drugs, or NSAIDs, are a group of medications commonly used to treat pain and conditions like arthritis. They reduce pain, inflammation and reduce fevers. NSAIDs commonly interact with other medications, but gastric bypass patients should also avoid using NSAIDs. NSAIDs increase the chances of getting a stomach ulcer, and these are much more difficult to treat in patients who have had gastric bypass. Common NSAIDs include:
- asprin
- ibuprofen
- Advil
- Motrin
- Aleve
- Naprosyn
- Vioxx
- Celebrex
Most bypass patients are prescribed medicines that help prevent ulcers.
- Non-steroidal anti-inflammatory drugs, or NSAIDs, are a group of medications commonly used to treat pain and conditions like arthritis.
- NSAIDs increase the chances of getting a stomach ulcer, and these are much more difficult to treat in patients who have had gastric bypass.
Consult Your Doctor
Dobbhoff Feeding Tube Vs. PEG
Learn More
As with any medication, it is important to consult with your doctor before starting. This becomes even more important after gastric bypass surgery 2. To be as healthy and successful as possible after gastric bypass, maintain regular follow- up appointments with both your bariatric surgeon and primary care physician. Your bariatric surgeon will likely conduct more in-depth blood work than your primary care physician, and his input and care is vital in ensuring your long-term success. In addition, follow-up with your primary care physician is important because he will likely need to adjust dosages of any maintenance medications you take, such as medicines for high blood pressure or diabetes.
- As with any medication, it is important to consult with your doctor before starting.
- In addition, follow-up with your primary care physician is important because he will likely need to adjust dosages of any maintenance medications you take, such as medicines for high blood pressure or diabetes.
Related Articles
References
- Obesity Action Coalition: I am a Bariatric Surgery Patient. Which Medications are Recommended and Which Ones Should I Avoid?
- Medline Plus: Gastric Bypass Surgery
- UCSF Medical Center: Life After Bariatric Surgery
- Beamish AJ, Reinehr T. Should bariatric surgery be performed in adolescents?Eur J Endocrinol. 2017 Apr;176(4):D1-D15. doi:10.1530/EJE-16-0906
- American Society for Metabolic and Bariatric Surgery. Bariatric Surgery Procedures.
- Maciejewski ML et al. Bariatric Surgery and Long-term Durability of Weight Loss JAMA Surg. 2016 Nov 1;151(11):1046-1055. doi:10.1001/jamasurg.2016.2317
- Telem DA, Jones DB, Schauer PR, Brethauer SA, Rosenthal RJ, Provost D, Jones SB. (March 2020). Society of American Gastrointestinal and Endoscopic Surgeons (SAGES). Updated Panel Report: Best Practices for the Surgical Treatment of Obesity.
- Stahl JM, Malhotra S. Obesity Surgery Indications and Contraindications. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019. Updated May 2020.
- Kim RB. (Updated April 2020). Bariatric operations for management of obesity: Indications and preoperative preparation. Jones D, ed. UpToDate. Waltham, MA: UpToDate.
- Palermo M, Acquafresca PA, Rogula T, Duza GE, Serr E. Late surgical complications after gastric by-pass: a literature review. Arq Bras Cir Dig. 2015 Apr-Jun; 28(2): 139–143. doi:10.1590/S0102-67202015000200014
- University of Rochester Medical Center. (2020). Anastomotic Leak After Gastric Bypass Surgery
- Kim RB. (Updated May 2019). Laparoscopic Roux-en-Y gastric bypass. Jones D, ed. UpToDate. Waltham, MA: UpToDate.
- Wolfe BM, Kvach E, Eckel RH. Treatment of Obesity: Weight Loss and Bariatric Surgery. Circ Res. 2016 May 27; 118(11): 1844–1855.doi:10.1161/CIRCRESAHA.116.307591
- Monpellier VM, Antoniou EE, Aarts EO, Janssen IMC, Jansen ATM. Improvement of Health-Related Quality of Life After Roux-en-Y Gastric Bypass Related to Weight Loss. Obes Surg. 2017; 27(5): 1168–1173. doi:10.1007/s11695-016-2468-6
- Adams TD, Mehta TS, Davidson LE, Hunt SC. All-Cause and Cause-Specific Mortality Associated with Bariatric Surgery: A Review. Curr Atheroscler Rep. 2015 Dec; 17(12): 74. doi:10.1007/s11883-015-0551-4
- John Hopkins Medicine. Roux-en-Y Gastric Bypass Weight-Loss Surgery.
- Edholm D, Kullberg J, Karlsson FA, Haenni A, Ahlström H, Sundbom M. Changes in liver volume and body composition during 4 weeks of low calorie diet before laparoscopic gastric bypass. Surg Obes Relat Dis. May-Jun 2015;11(3):602-6. doi:10.1016/j.soard.2014.07.018
- UCSF Health. Recovery from Bariatric Surgery.
- Richardson WS, Plaisance AM, Periou L, Buquoi J, Tillery D. Long-term Management of Patients After Weight Loss Surgery. Ochsner J. 2009 Fall; 9(3): 154–159.
- UPMC. (2020). About Post-Surgery Bariatric Vitamins & Bariatric Supplements.
- Aminiana A, Changa J, Brethauera SA, Kimb JJ, American Society for Metabolic and Bariatric Surgery Clinical Issues Committee. ASMBS updated position statement on bariatric surgery in class I obesity (BMI 30-35 kg/m2). Surgery for Obesity and Related Diseases. 14 (2018) 1071-87.
- UCLA Health. Obesity Treatments. Gastric Bypass Surgery.
Writer Bio
Derek Helderman is a Bariatric Registered Dietitian currently working in a nutrition counseling role. Helderman graduated summa cum laude from Southeast Missouri State and completed his dietetic internship at Vanderbilt University Medical Center in Nashville, Tenn.