What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
Dangerous Blood Oxygen Levels
In order to live, every cell in your body needs oxygen to properly function. Oxygen is a critical nutrient and the body can die within six minutes without it. Any level below 88 percent is dangerous and incapacitating to your body. High oxygen levels are important for overall good health.
Normal Levels
Healthy people usually have a blood oxygen level above 95 percent. Added oxygen may be needed for people whose oxygen level falls below 90 percent and home oxygen therapy may be recommended to regain normal levels. When oxygen saturation drops below 80 percent, severe hypoxemia occurs. Hypoxemia is a low level of oxygen in the blood that disrupts body function and harms vital tissues. It can be life-threatening in severe cases.
- Healthy people usually have a blood oxygen level above 95 percent.
Causes
Causes of Low Blood Oxygen Levels
Learn More
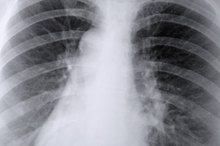
Anything that interferes with oxygen passing into your bloodstream and throughout your body can cause low blood oxygen. Low oxygen levels occur in people with respiratory disorders such as emphysema and chronic bronchitis, which are also known as chronic obstructive pulmonary disease. Lung cancer can cause low oxygen levels, as can cystic fibrosis and pulmonary fibrosis. Low oxygen levels can occur at night, disrupting sleep and devastating the cells’ ability to repair, cleanse and reproduce. The result is feeling exhausted in the morning and tired throughout the day.
- Anything that interferes with oxygen passing into your bloodstream and throughout your body can cause low blood oxygen.
- Low oxygen levels can occur at night, disrupting sleep and devastating the cells’ ability to repair, cleanse and reproduce.
Symptoms
Oxygen levels that are too low can result in muscle aches, obesity, headaches, lowered immunity, fatigue, circulation problems, anxiety, high blood pressure and depression. You may also experience more serious symptoms, including congestive heart failure, heart attack and stroke.
Detection
Causes of High Carbon Dioxide in the Blood
Learn More
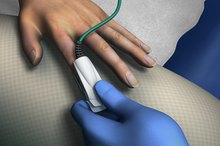
Oximetry testing provides valuable information about your oxygen levels. Testing the saturation levels of oxygen in the blood can be done while exercising, sitting and during an overnight period of eight hours.
Remedies
Natural ways to raise oxygen blood levels include eating foods high in complex carbohydrates; this increases your blood’s capability to transport oxygen to all your cells. Also, maintaining good posture helps your lungs take in more oxygen and high-impact exercise for 30 minutes every day--such as running and aerobics--increases the pathways of oxygen in your body.
Treatments
Natural ways to fight dangerous blood oxygen levels are to avoid fatty foods which lower oxygen-carrying capacity and to quit smoking, as cigarette smoke increases carbon dioxide in your blood. Avoiding bad posture also aids in the flow of oxygen throughout your body. Oxygen therapy is used to help normalize blood oxygen concentration, which helps your organs cleanse, heal and function correctly. After the therapy you may feel more energetic, rested and experience a greater sense of well-being and mental clarity after your oxygen levels are increased.
- Natural ways to fight dangerous blood oxygen levels are to avoid fatty foods which lower oxygen-carrying capacity and to quit smoking, as cigarette smoke increases carbon dioxide in your blood.
Related Articles
References
- Mayo Clinic
- McGill University, Office for Science and Society, "Under the Microscope: Blood"
- Collins JA, Rudenski A, Gibson J, Howard L, O'Driscoll R. Relating oxygen partial pressure, saturation and content: the haemoglobin-oxygen dissociation curve. Breathe (Sheff). 2015;11(3):194–201. doi: 10.1183/20734735.001415
- Gossman W, Alghoula F, Berim I. Anoxia (Hypoxic Hypoxia) [Updated 2019 Jul 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-.
- Giaccia AJ, Simon MC, Johnson R. The biology of hypoxia: the role of oxygen sensing in development, normal function, and disease. Genes Dev. 2004;18(18):2183–2194. doi: 10.1101/gad.1243304
- Leach RM, Treacher DF. Oxygen transport-2. Tissue hypoxia. BMJ. 1998;317(7169):1370–1373. doi: 10.1136/bmj.317.7169.1370
- Hafen BB, Sharma S. Oxygen Saturation. [Updated 2019 Jun 2]. In: StatPearls Treasure Island (FL): StatPearls Publishing. 2019 Jan.
Writer Bio
Charlotte Mission is an avid reader and writer. She has written professionally for over 5 years and for pleasure for many more. Her work has appeared on eHow.com and AssociatedContent.com. She is currently pursuing a degree in History.