What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
How to Heal Scars & Wounds
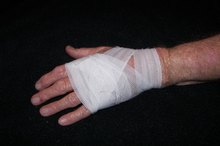
Scars and wounds, whether from an injury or as the result of a surgical procedure, must heal quickly and properly to minimize infection and scarring. That's why you should always pay close attention to your health care provider when she explains how to care for your wound. By cleaning and dressing a wound well, it should heal properly with minimal scarring. The American Academy of Dermatology notes that scarring is natural part of the healing process and usually improves on its own 1.
Clean the wound daily to avoid infection, Medline Plus advises 3. Make a saline solution by combining cup of warm water and a tsp. of salt and mix until dissolved. Pour the solution directly on the wound. You can also use an antibacterial soap. Lather up, and pat a small amount of the lather onto the wound, leaving the suds on it for 20 seconds. Then rinse the wound with cool water.
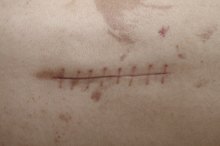
How to Care for a Surgical Scar
Learn More
Cover the wound only if it is in an area prone to getting dirty or where it could reopen because of your normal activities. Otherwise, the American Academy of Family Physicians suggests, leave the wound open to the air and keep it dry to help it to heal faster 2. Ask your health care provider whether you should leave the wound open or bandage it. Some larger wounds like scrapes and rashes heal better in a moist environment.
Keep your hands away from the wound. It can be tempting to touch, pick or peel at a scab or scar, but you can transfer germs and dirt from your hand into the opening of the wound. This leaves you susceptible to infection and swelling and a slower healing time, which can lead to scarring.
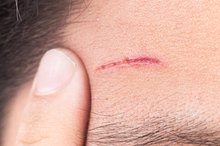
How Can I Make My Scratches Heal Fast?
Learn More
Watch for signs of infection, and report them to your doctor if you notice redness, pain, swelling or a milky liquid draining from the wound. Infection halts the healing process and can make you sick. You should talk to your doctor immediately so you can begin taking antibiotics to stop the infection and continue the healing process.
Apply silicone gel pads or cream to the healed wound site daily once the sore is no longer open. The American Academy of Dermatology says that silicone gels are an effective way to reduce scarring 1. Microdermabrasion, or exfoliating the scar with an abrasive material, can also help smooth the skin and reduce puffiness so that the scar is less noticeable and flush with the rest of your skin.
If your scar really bothers you, or heals badly, your dermatologist can talk to you about scar revision or laser resurfacing for smoother skin.
Related Articles
References
- American Academy of Dermatology: What Is a Scar?
- American Academy of Family Physicians: Cuts, Scrapes and Stitches
- Medline: Surgical Wound Care
- 3M Wound Resource Center. http://solutions.3m.co.uk/wps/portal/3M/en_GB/skin-care/wound-resource-centre/
- Mccaughan D, Sheard L, Cullum N, Dumville J, Chetter I. Patients' perceptions and experiences of living with a surgical wound healing by secondary intention: A qualitative study. Int J Nurs Stud. 2018;77:29-38. doi:10.1016/j.ijnurstu.2017.09.015
- Krafts KP. Tissue repair: The hidden drama. Organogenesis. 2010;6(4):225-33. doi:10.4161/org.6.4.12555
- Chetter IC, Oswald AV, Fletcher M, Dumville JC, Cullum NA. A survey of patients with surgical wounds healing by secondary intention; an assessment of prevalence, aetiology, duration and management. J Tissue Viability. 2017;26(2):103-107. doi:10.1016/j.jtv.2016.12.004
- Singh PK, Saxena N, Poddar D, et al. Comparative Study Of Wound Healing In Primary Versus Delayed Primary Closure In Contaminated Abdominal Surgery. Hellenic J Surg. 2016;88:314–320. doi:10.1007/s13126-016-0340-8
- Surgical Patient Education Program: Prepare for the Best Recovery. American College of Surgeons. 2018.
- Rushbrook JL, White G, Kidger L, Marsh P, Taggart TF. The antibacterial effect of 2-octyl cyanoacrylate (Dermabond®) skin adhesive. J Infect Prev. 2014;15(6):236-239. doi:10.1177/1757177414551562
- Lazar HL, Mccann J, Fitzgerald CA, Cabral HJ. Adhesive strips versus subcuticular suture for mediansternotomy wound closure. J Card Surg. 2011;26(4):344-7. doi:10.1111/j.1540-8191.2011.01257.x
- 3M Wound Resource Center.
Writer Bio
Kay Ireland specializes in health, fitness and lifestyle topics. She is a support worker in the neonatal intensive care and antepartum units of her local hospital and recently became a certified group fitness instructor.