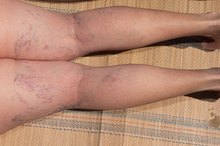
Knees & Ankles Turn Purple After Running
Discoloration in the legs after exercise may be associated with having a condition known as peripheral artery disease, or PAD 1. This circulatory disorder affects the limbs, depriving them of proper blood flow and oxygen. In many cases, symptoms can appear and may be worse after exercise.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
What Is PAD?
Peripheral artery disease develops in the arms and legs because of plaque buildup in the arteries, causing them to harden and restrict blood flow 1. PAD, or atherosclerosis, also affects the arteries in the brain and heart and is the primary reason for an individual having a stroke or heart attack. If you have PAD, your chance of experiencing a stroke or heart attack is significantly higher, according to Dr. Michael Jaff of Massachusetts General Hospital. Additionally, if you are older than 50 and diabetic or smoke cigarettes, your risk factor is one in three of developing PAD. PAD can cause your legs to bother you when you are active, as in running, walking or other exercise. You may experience pain and reddish-purple discoloration of the skin, a sign of poor circulation. The symptoms of PAD are often missed by many doctors and mistaken for general signs of aging, arthritis in the spine, or problems with the hips.
- Peripheral artery disease develops in the arms and legs because of plaque buildup in the arteries, causing them to harden and restrict blood flow 1.
- PAD, or atherosclerosis, also affects the arteries in the brain and heart and is the primary reason for an individual having a stroke or heart attack.
Testing and Diagnosis
Causes of Fatigue & Aching Legs
Learn More
Testing for PAD is usually non-invasive and safe. A specialist will start by taking your blood pressure in both arms and legs to determine if there is a difference in pressure in one or more areas. Once testing is completed, treatment consists of medication, specific exercises designed to stimulate blood flow and possible minimally invasive procedures to aid in restoring circulation to your legs.
Symptoms
Narrowing of the arteries and restriction of blood flow can cause cramping pain in the legs; discoloration of the skin; muscle pain in the thighs, calves and feet especially during and after exercise; numbness; and coldness in the legs and feet. Additionally, PAD may be associated with Raynaud's phenomenon where blood flow is severely restricted to the capillaries in the toes and feet, causing extreme pain and skin discoloration ranging from white to blue and blackish-purple.
The pain in your legs caused by PAD is usually intermittent, where it comes and goes, and is one of the more prominent symptoms leading to a diagnosis of PAD. You may experience the pain as fatigue, aching, burning or general discomfort. These symptoms usually disappear when you elevate your legs and rest and return with an increase in exercise. The calf muscle is where you will feel symptoms most often.
- Narrowing of the arteries and restriction of blood flow can cause cramping pain in the legs; discoloration of the skin; muscle pain in the thighs, calves and feet especially during and after exercise; numbness; and coldness in the legs and feet.
- The pain in your legs caused by PAD is usually intermittent, where it comes and goes, and is one of the more prominent symptoms leading to a diagnosis of PAD.
Advanced Symptoms
Symptoms of Poor Circulation in the Legs
Learn More
If you notice that you're experiencing pain in your legs even when you lie down and rest, you may be suffering from advanced PAD or ischemic rest pain. It is typically brought on by severe blockage of blood flow to your tissues. Symptoms include pain that is worse when your legs are elevated but better when you allow them to hang down over the side of a chair. Additionally, you may experience tingling and pain in your feet and toes that is made worse even by the touch of the sheets when you lie in bed. Additional symptoms leading to a diagnosis of ischemic rest pain are hair loss on your feet and toes, shiny, tight skin, withered calf muscles and thickened toenails. If you experience these symptoms, you may also be at risk for blood clots, leg ulcers and gangrene.
- If you notice that you're experiencing pain in your legs even when you lie down and rest, you may be suffering from advanced PAD or ischemic rest pain.
- Additionally, you may experience tingling and pain in your feet and toes that is made worse even by the touch of the sheets when you lie in bed.
Treatment
The most important lifestyle change you can implement to overcome PAD is to include regular, specific exercise into your daily routine. Those exercises should enhance your cardiovascular system and improve the flow of blood to your legs. Walking is noted as the best form of exercise for people with PAD by the University of Maryland Medical Center. However, for people who experience pain and other symptoms because of walking, upper body aerobic exercise is recommended. It stimulates blood flow in the body and helps to oxygenate the blood, relieving pain in the arms and legs.
- The most important lifestyle change you can implement to overcome PAD is to include regular, specific exercise into your daily routine.
- However, for people who experience pain and other symptoms because of walking, upper body aerobic exercise is recommended.
Related Articles
References
Writer Bio
Jean Bardot is a freelance writer and natural health practitioner. She started writing in 1994 and has contributed articles to publications such as "Similimum" and the "IFH Journal." She has a Bachelor of Science in public health from the University of North Carolina and a Master of Science in holistic nutrition from Clayton College of Natural Health.