Does a Hernia Belt Really Help?
A hernia is a protrusion or bulge of an organ through surrounding tissue, usually in the abdominal wall. It can be in the groin or at the site of previous abdominal surgery. Groin or inguinal hernias are very common. The bulge is usually small intestine or intra-abdominal fat that protrudes through a weakness between the muscles of the abdominal wall.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Hernia Belts
A hernia belt compresses the abdominal wall to force the protrusion back into the abdomen--in medical terms, to become “reduced." A hernia that cannot be reduced is said to be incarcerated ("stuck"). Occasionally such hernias can become strangulated, cutting off the blood supply to the area that is bulging. Without emergency surgery, a serious infection can follow.
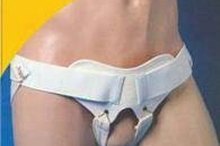
Hernia belts are usually elastic, applied around the abdomen to keep the hernia from bulging. A truss is a special kind of hernia belt that is meant to prevent bulging of a groin hernia. It has a plate of metal or hard plastic that lies over the area of the hernia and applies pressure to prevent the bulge from protruding. A hernia belt is not necessary if the patient has no symptoms.
Although a hernia belt will keep the bulge in the reduced position, it must be worn at all times, or the bulge will recur with such simple activities as coughing, sneezing or straining during a bowel movement. For the vast majority of patients with hernias, a hernia belt is an unsatisfactory solution, because it does not provide a cure and can be very uncomfortable. In addition, hernia belts can weaken the tissues further because of the constant pressure. This is particularly true with a truss, which exerts more pressure.
A hernia doesn't always require surgery. In 2006, the Journal of the American Medical Association carried a report on a study by Dr. Robert J. Fitzgibbons Jr. and colleagues 1. It showed that asymptomatic men with groin hernias can safely be observed without surgery because the risk of complications is very small. However, hernia surgery is safe for nearly all patients. Hernia belts are recommended only for the occasional extremely high-risk, symptomatic patient who might not even tolerate surgery under local anesthesia.
- A hernia belt compresses the abdominal wall to force the protrusion back into the abdomen--in medical terms, to become “reduced."
- For the vast majority of patients with hernias, a hernia belt is an unsatisfactory solution, because it does not provide a cure and can be very uncomfortable.
Related Articles
References
- JAMA. Watchful Waiting vs Repair of Inguinal Hernia in Minimally Symptomatic Men A Randomized Clinical Trial Robert J. Fitzgibbons et al. 2006;295:285-292.
- Yoong P, Duffy S, Marshall TJ. The inguinal and femoral canals: A practical step-by-step approach to accurate sonographic assessment. Indian J Radiol Imaging. 2013;23(4):391–395. doi:10.4103/0971-3026.125586
- Harvard Health Publishing. Inguinal hernia. Updated July 2019.
- Lee SS, Jung HJ, Park BS, Son GM, Cho YH. Surgical Aspects of Recurrent Inguinal Hernia in Adults. Am Surg. 2016;82(11):1063–1067.
- Wang KS. Assessment and management of inguinal hernia in infants. Pediatrics. 2012;130(4):768-73. doi:10.1542/peds.2012-2008
- University of California San Francisco General Surgery. Inguinal hernia.
- National Institute of Diabetes and Digestive and Kidney Diseases. Inguinal hernia. Updated September 2019.
- Kulacoglu H. Current options in inguinal hernia repair in adult patients. Hippokratia. 2011;15(3):223–231.
- National Health Services. Inguinal hernia repair recovery. Updated June 14, 2018.
- Hernia. National Institutes of Health.