Menopause & Eczema
Menopause brings with it a time of change and upheaval. As ovulation ceases and estrogen production drops, women may experience a number of symptoms, such as hot flashes, mood swings and hair loss. Women may also notice changes in their skin. Hormonal fluctuations affect the skin and may cause an itchy skin condition called eczema.
Eczema
The term eczema describes any type of itchy skin rash. The broad term of eczema includes atopic dermatitis, contact dermatitis, seborrheic dermatitis, and other rashes. Eczema may be caused by an allergy, repeated exposure to an irritant, such as a soap or detergent, inherited predisposition or an overactive immune system.
Effect of Menopause
Dyshidrotic Eczema and Menopause
Learn More
Menopause occurs when the ovaries stop producing the hormone estrogen. During the time leading up to menopause, hormone levels fluctuate, which causes the symptoms typically associated with menopause, for example, hot flashes and mood changes 23. Declining estrogen levels also affect the skin. Collagen, a fibrous protein that supports the skin, loses strength and effectiveness as estrogen levels fall. Additionally, the sebaceous glands of the skin produce less lubricating oils and the skin is unable to retain moisture. The skin becomes dry and itchy 2. The immune system may become less active during menopause, lowering the body’s resistance to irritants and allergens 3.
Signs
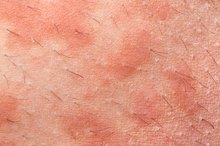
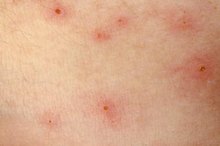
Eczema appears as itchy, red patches on the skin. Although the itch is intense, it may fade periodically. The skin may appear swollen and inflamed even when you do not scratch. Some areas may swell and crack, releasing a clear fluid. Skin rashes associated with menopause tend to occur mostly on the face, especially the forehead and nose or on the neck, back, chest, arms and legs 3.
- Eczema appears as itchy, red patches on the skin.
- The skin may appear swollen and inflamed even when you do not scratch.
Treatment
Follicular Eczema
Learn More
Menopause-associated eczema may be treated with over-the-counter creams. The creams help return moisture to dry skin and relieve symptoms, but they will not cure the eczema. Prescription-strength lotions containing topical corticosteroids relieve more intense itching and help control inflammation. Oral corticosteroids are prescribed for severe rashes. Topical or oral antibiotics may be necessary if an infection develops. Hormone replacement therapy helps relieve some menopause symptoms, but it may be associated with serious side effects, including an increased risk of breast cancer 26.
- Menopause-associated eczema may be treated with over-the-counter creams.
Coping
Taking lukewarm showers can help relieve the intense itching associated with eczema. Use mild soaps and dry your skin gently to avoid further irritation. Use moisturizers regularly to maintain skin moisture and drink plenty of water.
Related Articles
References
- DermaNetNZ: Menopause and the Skin
- AtoZMenopause.com: Itchy Skin Rash During Menopause
- EczemaNet: What Is Eczema?
- American Cancer Society: Menopausal Hormone Replacement Therapy and Cancer Risk
- Murota H, Yamaga K, Ono E, Murayama N, Yokozeki H, Katayama I. Why does sweat lead to the development of itch in atopic dermatitis?. Exp Dermatol. 2019;28(12):1416-1421. doi:10.1111/exd.13981
- David Boothe W, Tarbox JA, Tarbox MB. Atopic dermatitis: Pathophysiology. Adv Exp Med Biol. 2017;1027:21-37. doi:10.1007/978-3-319-64804-0_3
- US National Library of Medicine, Genetics Home Reference. FLG gene. Filaggrin. Updated January 21, 2020.