What Parents Should Know About Normal Blood Sugar Levels for Toddlers
You're probably used to your toddler's dramatic mood shifts and changes in energy. Often, these changes are just toddlers being toddlers. But if irritability and fatigue are accompanied by other symptoms, it can be a possible sign of childhood diabetes.
Here's what you need to know about normal blood sugar levels in children — and what to do if you notice signs that your child might have diabetes 2.**
Normal Blood Sugar Levels in Toddlers
Blood sugar, or glucose, is the body's main form of energy. The body mainly gets glucose by metabolizing the carbohydrates in food. But people with diabetes have blood sugar levels that are too high, a condition known as hyperglycemia. This can have both short- and long-term health consequences.
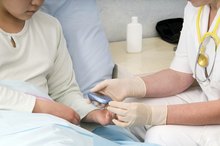
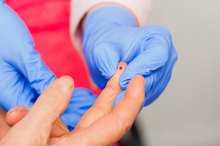
There are several different blood tests that measure blood sugar levels and check for diabetes. Two of them — a random blood sugar test and a hemoglobin A1C test — can be performed during your regular visit to the pediatrician. A random blood sugar test measures your toddler's blood sugar at that moment, while an A1C test measures his or her average blood sugar level over the last three months.
According to Yale School of Medicine, normal blood sugars for toddlers at certain times of the day are as follows 1:
- Before breakfast (fasting blood sugar): 70 to 120 mg/dL
- One to two hours after meals: Less than 140 mg/dL
- Before meals and at bedtime: 70 to 120 mg/dL
A normal A1C level in children is 6.5, according to the Mayo Clinic 23.** If your child's blood sugar levels are elevated, your pediatrician might prescribe other blood or urine tests to get a diagnosis.
Read more: What Parents Should Know About Normal Blood Sugar Levels for Kids
- Blood sugar, or glucose, is the body's main form of energy.
- If your child's blood sugar levels are elevated, your pediatrician might prescribe other blood or urine tests to get a diagnosis.
When Should Your Toddler Get Tested for Diabetes?
What Are the Signs & Symptoms of Blood Sugar Problems in Children?
Learn More
Recognizing the symptoms of diabetes in toddlers can be challenging, because they can't always articulate their symptoms to you. There are two main forms of diabetes in children — type 1 and type 2 23.** In order to recognize the symptoms, it's helpful to first understand a bit more about how the body normally manages blood sugar, and how the two different types of diabetes affect this system.
After the body metabolizes carbs into glucose, insulin — a hormone produced by the pancreas — helps move the glucose out of the blood and into the cells, which use it for energy. While insulin is removing glucose from the blood, it is also lowering blood sugar levels.
Read more: Why Too High or Too Low Blood Sugar Could Be Dangerous
People with type 1 diabetes are said to be insulin deficient, meaning that their pancreases don't make enough insulin. Without enough insulin, glucose builds up in the blood, causing hyperglycemia. This type of diabetes is heritable, meaning that it is partially caused by genetics, but there are other things that influence its development. "Type 1 can develop at any age, but it's more typical in children," says Heidi Quinn, RDN, a certified diabetes educator at Harvard's Joslin Diabetes Center 234.**
Type 1 diabetes usually develops in children and tweens aged 4 to 6 and 10 to 14, according to Stanford Children's Health 23. Therefore, while diabetes can occur in toddlers, it is more common in slightly older children 2.
In the case of type 2 diabetes, the body makes enough insulin, but the cells don't respond properly to its effects — a condition known as insulin resistance. This results in high blood sugar, according to the Joslin Diabetes Center 4.**
Read more: 5 Healthy Habits That Can Keep Blood Sugar in Check During Pregnancy
Type 2 diabetes is partially genetic, but it's not as heritable as type 1 4.** Though the exact causes are currently unknown, type 2 has been connected to environmental factors such as poor diet and obesity. "Type 2 diabetes is more common in adults," says Quinn, "but we're seeing it more in younger ages now, due to the obesity epidemic. 4"
The symptoms of type 1 and type 2 diabetes are similar, but they develop much more quickly in type 1, says Quinn 2.** Here's what you should look out for, according to Stanford Children's Health 3:
- Frequent urination (especially within a short time frame)
- Unusual/excessive thirst
- Extreme hunger accompanied by weight loss
- Irritability and mood changes
- Fatigue
- Eye rubbing (untreated diabetes can cause blurry vision)
- Nausea and vomiting
- Fruity-smelling breath
- Rapid breathing
Many of these symptoms — such as mood changes and fatigue — are common in young children. But if these symptoms occur with other signs of diabetes, see your toddler's doctor. If left untreated, diabetes (particularly type 1) can become life-threatening.
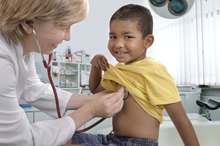
As Quinn says, type 2 diabetes develops more slowly, meaning that it can be more easily diagnosed at your child's regular doctor appointment. Also, it's important to note that overweight children are at a higher risk for type 2 diabetes than kids who have a normal weight 23.**
- Recognizing the symptoms of diabetes in toddlers can be challenging, because they can't always articulate their symptoms to you.
- Read more: Why Too High or Too Low Blood Sugar Could Be Dangerous People with type 1 diabetes are said to be insulin deficient, meaning that their pancreases don't make enough insulin.
Managing Your Toddler's Diabetes
Managing your toddler's diabetes — and eventually teaching children how to manage it on their own — is critical for their long-term health 23.** Over time, poorly controlled blood sugar can cause:
- damage to the eyes
- kidneys
- nerves
- heart
- blood vessels
- according to KidsHealth 6
Related Articles
References
- Mayo Clinic: "Type 1 Diabetes in Children"
- Stanford Children's Health: "Type 1 Diabetes Mellitus in Children"
- Joslin Diabetes Center: "What Is Type 2 Diabetes?"
- American Diabetes Association: "Hypoglycemia (Low Blood Sugar)"
- Centers for Disease Control and Prevention. Diabetes and pregnancy: Gestational diabetes.
- Zisser HC, Bevier W, Dassau E, Jovanovic L. Siphon effects on continuous subcutaneous insulin infusion pump delivery performance. J Diabetes Sci Technol. 2010;4(1):98-103. doi:10.1177/193229681000400112
- Lakhtakia R. The history of diabetes mellitus. Sultan Qaboos Univ Med J. 2013;13(3):368-370. doi:10.12816/0003257
- Bryan Bledsoe, DO, FACEP, FAAEM, EMT-P. Journal of Emergency Medical Service. What's the difference between diabetes mellitus and diabetes insipidus.
- American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care. 2014;37(Supplement 1):S81-S90. doi:10.2337/dc14-S081
- Center for Disease Control and Prevention. Prediabetes - your chance to prevent diabetes. Updated June 11, 2020.
- Center for Disease Control and Prevention. Type 2 diabetes. Updated: May 30, 2019.
- Centers for Disease Control and Prevention. Diabetes during pregnancy. Updated: June 12, 2018.
- Centers for Disease Control and Prevention. Diabetes and pregnancy: Gestational diabetes.
- Laugesen E, Østergaard JA, Leslie RD; Danish Diabetes Academy Workshop and Workshop Speakers. Latent autoimmune diabetes of the adult: current knowledge and uncertainty [published correction appears in Diabet Med. 2015 Dec;32(12):1670]. Diabet Med. 2015;32(7):843-852. doi:10.1111/dme.12700
- National Institute of Diabetes and Digestive and Kidney Disease. Monogenic diabetes (neonatal diabetes mellitus & MODY). Updated November, 2017.
- Lemelman MB, Letourneau L, Greeley SAW. Neonatal diabetes mellitus: An update on diagnosis and management. Clin Perinatol. 2018;45(1):41-59. doi:10.1016/j.clp.2017.10.006
- American Diabetes Association. Complications.
- American Diabetes Association. Diagnosis.
- American Diabetes Association. Eye exams for people with diabetes.
- Powers, MA. et. al. Diabetes self-management education and support in type 2 diabetes: A joint position statement of the American Diabetes Association, the American Association of Diabetes Educators, and the Academy of Nutrition and Dietetics. Diabetes Care. 2015;38 (7) 1372-1382; doi:10.2337/dc15-0730
- Association of Diabetes Care and Education Specialists. How a diabetes care and education specialist can help you.
- Bluml, BM, Kolb, L, Lipman, R. Evaluating the impact of year-long, augmented diabetes self-Management support. Popul Health Manag. 2019;22(6):522-528 doi:10.1089/pop.2018.0175