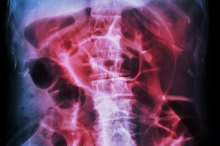
Colonoscopy Symptoms of a Perforated Colon
Colonoscopy is a test that enables the inspection of the entire colon using a fiberoptic tube known as colonoscope. A colonoscopy is used to detect abnormalities in the colon such as colon cancer and inflammation. Colon perforation occurs when the colonoscope punctures the wall of the colon during a colonoscopy 2. Emedtv.com states that risk of colon perforation is increased in patients with existing colon abnormalities 2. Patients should be aware of symptoms of colon perforation
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Bleeding
The National Institutes of Health states that bleeding from colon perforation may occur immediately after a colonoscopy or even several days later 123. Patients may notice bright red blood in the stool or notice blood trickling down the anus as they defecate. Patients may also experience severe weakness and dizziness upon standing. Patients should contact the doctor immediately when they notice signs of bleeding in the colon. They may require surgery to fix the colon perforation. Patients who have lost massive amounts of blood may require blood transfusions.
- The National Institutes of Health states that bleeding from colon perforation may occur immediately after a colonoscopy or even several days later 1.
- Patients who have lost massive amounts of blood may require blood transfusions.
Sepsis
Diverticulitis & Colonoscopy
Learn More
Perforation of the colon results in a hole in the bowel that allows bowel contents to enter the bloodstream and circulate to the rest of the body, resulting in a blood infection known as sepsis. Patients with sepsis due to colon perforation may experience fever, chills, shaking, confusion, rapid pulse and delirium. Sepsis is a serious illness that requires hospitalization in the intensive care unit.
Secondary Peritonitis
According to the National Institutes of Health, a perforated colon may result in a condition known as secondary peritonitis 13. Secondary peritonitis is the inflammation of the peritoneum, which are tissues that cover the colon and other abdominal organs 3. Peritonitis occurs when bacteria enter the peritoneum through the hole in colon. Signs and symptoms of peritonitis include fever, shaking chills, abdominal tenderness and a firm board-like abdomen.
Abdominal Pain and Distension
List of Foods for Diverticulitis
Learn More
According to the National Institutes of Health, patients with colon perforation may experience severe abdominal pain at the site of colon puncture 13. The abdominal pain may be aggravated by bending or lifting heavy objects. Abdominal distension may be caused by the pooling of blood in the colon and the surrounding regions due to colon perforation.
- According to the National Institutes of Health, patients with colon perforation may experience severe abdominal pain at the site of colon puncture 1.
- Abdominal distension may be caused by the pooling of blood in the colon and the surrounding regions due to colon perforation.
Related Articles
References
- The National Institutes of Health: Management of Complications of Colonoscopy
- Emedtv.com: Bowel Perforation during Colonoscopy
- The National Institutes of Health: Secondary Peritonitis
- Jones MW, Zabbo CP. Bowel Perforation. StatPearls Publishing. Updated February 22, 2019.
- Doklestić SK, Bajec DD, Djukić RV, et al. Secondary peritonitis - evaluation of 204 cases and literature review. J Med Life. 2014;7(2):132-8.
- Yamauchi A, Kudo SE, Mori Y, et al. Retrospective analysis of large bowel obstruction or perforation caused by oral preparation for colonoscopy. Endosc Int Open. 2017;5(6):E471-E476. doi:10.1055/s-0043-106200
- Navaneethan U, Kochhar G, Phull H, et al. Severe disease on endoscopy and steroid use increase the risk for bowel perforation during colonoscopy in inflammatory bowel disease patients. J Crohns Colitis. 2012;6(4):470-5. doi:10.1016/j.crohns.2011.10.005
- Banaszkiewicz Z, Woda Ł, Tojek K, Jarmocik P, Jawień A. Colorectal cancer with intestinal perforation - a retrospective analysis of treatment outcomes. Contemp Oncol (Pozn). 2014;18(6):414-8. doi:10.5114/wo.2014.46362
- Holmer C, Mallmann CA, Musch MA, Kreis ME, Gröne J. Surgical management of iatrogenic perforation of the gastrointestinal tract: 15 years of experience in a single center. World J Surg. 2017;41(8):1961-1965. doi:10.1007/s00268-017-3986-7
- Fontana T, Falco N, Torchia M, Tutino R, Gulotta G. Bowel perforation in Crohn's Disease: correlation between CDAI and Clavien-Dindo scores. G Chir. 2017;38(6):303-312. doi:10.11138/gchir/2017.38.6.303
- Lin XK, Wu DZ, Lin XF, Zheng N. Intestinal perforation secondary to ingested foreign bodies: a single-center experience with 38 cases. Pediatr Surg Int. 2017;33(5):605-608. doi:10.1007/s00383-017-4075-6
- Mukhopadhyay M. Intestinal injury from blunt abdominal trauma: a study of 47 cases. Oman Med J. 2009;24(4):256-9. doi:10.5001/omj.2009.52
- Shah R, Witt D, Asif T, Mir FF. Ipilimumab as a Cause of Severe Pan-Colitis and Colonic Perforation. Cureus. 2017;9(4):e1182. doi:10.7759/cureus.1182
- Lohsiriwat V. Colonoscopic perforation: incidence, risk factors, management and outcome. World J Gastroenterol. 2010;16(4):425-30. doi:10.3748/wjg.v16.i4.425
- Kothari K, Friedman B, Grimaldi GM, Hines JJ. Nontraumatic large bowel perforation: spectrum of etiologies and CT findings. Abdom Radiol (NY). 2017;42(11):2597-2608. doi:10.1007/s00261-017-1180-x
- Schmidt A, Fuchs KH, Caca K, Küllmer A, Meining A. The Endoscopic Treatment of Iatrogenic Gastrointestinal Perforation. Dtsch Arztebl Int. 2016;113(8):121-8. doi:10.3238/arztebl.2016.0121
- Levack MM, Madariaga ML, Kaafarani HM. Non-operative successful management of a perforated small bowel diverticulum. World J Gastroenterol. 2014;20(48):18477-9. doi:10.3748/wjg.v20.i48.18477
- Holmer, C., Mallmann, C., Musch, M., Kreis, M., and J. Grone. Surgical Management of Iatrogenic Perforation of the Gastrointestinal Tract: 15 Years of Experience in a Single Center. World Journal of Surgery. 2017 Mar 21. (Epub ahead of print).
- Kim, J., Lee, H., Ye, B. et al. Incidence of and Risk Factors for Free Bowel Perforation in Patients with Crohn’s Disease. Digestive Diseases and Sciences. 2017. 62(6):1607-1614.
- Kothari, K., Friedman, B., Grimaldi, G., and J. Hines. Nontraumatic Large Bowel Perforation: Spectrum of Etiologies and CT Findings. Abdominal Radiology. 2017 May 10. (Epub ahead of print).
- Yamauchi, A., Kudo, S., Mori, Y. et al. Retrospective Analysis of Large Bowel Obstruction or Perforation Caused by Oral Preparation for Colonoscopy. Endoscopy International Open. 2017. 5(6): E471-E476.
Writer Bio
Esther Kinuthia is a registered nurse with extensive experience in health and wellness. She holds a B.S. in nursing, B.A in psychology and has worked for more than ten years in the health-care field. She enjoys writing articles on a variety of topics for the Internet. Her work has been published in various websites.