Does Drinking Beer Exacerbate Nummular Dermatitis?
Chronic skin rashes such as nummular dermatitis, also called discoid or nummular eczema, cause discomfort and embarrassment 2. This skin condition, which produces coin-shaped lesions on the skin, affects around two in 1,000 people in the United States, according to the American Academy of Dermatology. Drinking alcohol in any form, including beer, can exacerbate nummular dermatitis.
Causes
Men develop nummular dermatitis more frequently than women, with the first outbreak often occurring between ages 55 and 65. Women more often develop the disorder between 15 and 25. Dry skin, a history of eczema or poor circulation to the legs can indicate a higher risk. An allergy to nickel, rubber or formaldehyde, and taking certain medications -- such as interferon, isoretinoin or neomycin -- have also been shown to increase susceptibility. In rare cases, mercury fillings appear to cause nummular dermatitis. A lesion may begin at the site of a minor skin injury, such as an insect bite.
- Men develop nummular dermatitis more frequently than women, with the first outbreak often occurring between ages 55 and 65.
- Women more often develop the disorder between 15 and 25.
Symptoms
Dry Flaking on the Nose
Learn More
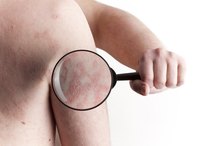
Nummular dermatitis starts as small reddened areas or blisters that grow together to form a coin-shaped or oval patch measuring between 1 and 4 inches in diameter. The lesions often appear on the legs, but can also appear on the back, arms, hands or other parts of the torso and may itch and burn. Over time, the center area may clear, giving the impression of a ringworm-like skin rash. The skin becomes flaky or scaly and may turn pink or brown. A discolored area often remains even after the lesions disappear, which can take up to a year or more.
- Nummular dermatitis starts as small reddened areas or blisters that grow together to form a coin-shaped or oval patch measuring between 1 and 4 inches in diameter.
- A discolored area often remains even after the lesions disappear, which can take up to a year or more.
Alcohol and Nummular Dermatitis
Heavy alcohol use can exacerbate or cause many types of skin lesions. Nummular dermatitis appears more frequently in people who abuse alcohol or drink heavily, especially in those who have abnormal liver function tests, which occur when alcohol damages the liver cells. People with this condition should consult their doctors about the risks of drinking alcohol.
Treatment
Causes of a Red Nose
Learn More
No medications are guaranteed to clear up this skin condition, which is why avoiding substances that can make it worse, such as alcohol, is so important. Steroid creams, moisturizing the skin, avoiding dry heat, humidifying the air -- especially in the winter months, when outbreaks often occur -- can help control or heal the lesions. Ultraviolet treatments several times a week over several months may help in some cases. Antibiotics can help if a secondary bacterial infection develops at the site.
- No medications are guaranteed to clear up this skin condition, which is why avoiding substances that can make it worse, such as alcohol, is so important.
- Steroid creams, moisturizing the skin, avoiding dry heat, humidifying the air -- especially in the winter months, when outbreaks often occur -- can help control or heal the lesions.
Related Articles
References
- The Merck Manual Home Health Book: Dermatitis
- DermNet NZ: Discoid Eczema
- DermNet NZ: Cutaneous Adverse Effects of Alcohol
- Other Dermatitis Conditions. Johns Hopkins Medicine.
- Nummular Eczema. US National Library of Medicine. April 2019.
- Nummular Eczema. American Osteopathic College of Dermatology.
- Nummular Eczema. Causes. American Academy of Dermatology Association.
- Lazzarini R, Duarte I, Ferreira AL. Patch tests. An Bras Dermatol. 2013;88(6):879-88. doi:10.1590/abd1806-4841.20132323
- Poudel RR, Belbase B, Kafle NK. Nummular eczema. J Community Hosp Intern Med Perspect. 2015;5(3):27909. doi:10.3402/jchimp.v5.27909
- Eczema. Harvard Medical School. February 2019.
- Berke R, Singh A, Guralnick M. Atopic dermatitis: an overview. Am Fam Physician. 2012;86(1):35-42.
- Coondoo A, Phiske M, Verma S, Lahiri K. Side-effects of topical steroids: A long overdue revisit. Indian Dermatol Online J. 2014;5(4):416-25. doi:10.4103/2229-5178.142483
- Tacrolimus & Pimecrolimus. American Osteopathic College of Dermatology.
- FDA approves Eucrisa for eczema. US Food & Drug Administration. December 2016.
- Kim WJ, Ko HC, Kim MB, Kim DW, Kim JM, Kim BS. Features of Staphylococcus aureus colonization in patients with nummular eczema. Br J Dermatol. 2013;168(3):658-60. doi:10.1111/j.1365-2133.2012.11072.x
- Eczema. TeensHealth from Nemours. September 2019.
- Coondoo A, Phiske M, Verma S, Lahiri K. Side-effects of topical steroids: A long overdue revisit 400. Indian Dermatol Online J. 2014;5(4):416-25. doi:10.4103/2229-5178.142483
- Schneider L, Tilles S, Lio P, et al. Atopic dermatitis: a practice parameter update 2012. J Allergy Clin Immunol. 2013;131(2):295-9.e1-27. doi:10.1016/j.jaci.2012.12.672
- Todorova A., Bruckbauer H., Ring J. (2015) Nummular Eczema. In: Katsambas A., Lotti T., Dessinioti C., D'Erme A. (eds) European Handbook of Dermatological Treatments. Springer, Berlin, Heidelberg
Writer Bio
A registered nurse with more than 25 years of experience in oncology, labor/delivery, neonatal intensive care, infertility and ophthalmology, Sharon Perkins has also coauthored and edited numerous health books for the Wiley "Dummies" series. Perkins also has extensive experience working in home health with medically fragile pediatric patients.