What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
The labia minora are the two folds of smooth, pigmented skin that lie within the larger labia majora and protect the entrance to the vagina. They are also a common site for the genital herpes lesions that, according to the Centers for Disease Control and Prevention (CDC), affect approximately one in five adult women in the United States 1. Herpes symptoms on the labia minora can be difficult to distinguish from those produced by other kinds of infections, therefore culture and/or antigen testing for the herpes simplex virus is required for definitive diagnosis.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Blisters
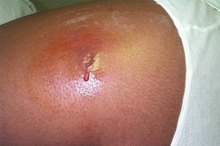
The characteristic lesion of herpes, according to Cernik, Gallina and Brodell's 2008 report in the “Archives of Internal Medicine,” is a painful 1 to 2 mm bump or blister with a central depression or dimple 3. Blisters on the labia minora often develop in clusters and rupture spontaneously, releasing clear or cloudy straw-colored fluid that is highly infectious. Blisters may be distributed on one or both sides of the labia minora. Blisters that occur on both sides are sometimes referred to as “kissing lesions."
- The characteristic lesion of herpes, according to Cernik, Gallina and Brodell's 2008 report in the “Archives of Internal Medicine,” is a painful 1 to 2 mm bump or blister with a central depression or dimple 3.
Ulcers
How Long Does an Outbreak of Genital Warts Last?
Learn More
Women often fail to recognize ulcers as a symptom of genital herpes 1. The ulcer that appears on the labia minora and other parts of the female external genitalia is commonly described as a “punched-out” lesion, according to Dr. Lawrence Corey in “Harrison’s Principles of Internal Medicine,” because of its well-defined borders. Ulcers are usually larger than blisters and appear as uniform, shallow, dark pink or red erosions which make urination extremely painful.
Crusts
Some blisters and ulcers develop crusts three to four days after they appear, according to Cernik and colleagues' 2008 article in the “Archives of Internal Medicine.” Crusts resemble a soft, crumbly or sandy scab which, like sand, is often discernibly yellow. As lesions crust over, they frequently become extremely itchy.
Related Articles
References
- CDC: Genital Herpes--CDC Fact Sheet
- “Harrison’s Principles of Internal Medicine, 17th edition;” A.S. Fauci, E. Braunwald, D.L. Kasper, S.L. Hauser, D.L. Longer, J.L. Jameson and J. Loscalzo (Eds.); 2008
- “Archives of Internal Medicine;” The Treatment of Herpes Simplex: An Evidence-Based Review; C. Cernik, K. Gallina and R.T. Brodell; June 2008
- Barrett MM, Carlson JA. A clinicopathologic study of labia minora hypertrophy: signs of localized lymphedema were universal. J Low Genit Tract Dis. 2014;18(1):13-20. doi:10.1097/LGT.0b013e31828d3989
- Gowda AU, Chopra N, Khalifeh M. Indications, Techniques and Complications of Labiaplasty. Eplasty. 2015;15:ic46.
- Coutant-foulc P, Lewis FM, Berville S, et al. Unilateral vulval swelling in cyclists: a report of 8 cases. J Low Genit Tract Dis. 2014;18(4):e84-9. doi:10.1097/LGT.0000000000000027
- Pandey D, Shetty J, Saxena A, Srilatha PS. Leiomyoma in vulva: a diagnostic dilemma. Case Rep Obstet Gynecol. 2014;2014:386432. doi:10.1155/2014/386432
Writer Bio
Heather Gloria began writing professionally in 1990. Her work has appeared in several professional and peer-reviewed publications including "Nutrition in Clinical Practice." Gloria earned both a Bachelor of Science in food science and human nutrition from the University of Illinois. She also maintains the "registered dietitian" credential and her professional interests include therapeutic nutrition, preventive medicine and women's health.