Causes of Red Swollen Feet & Ankles
Swelling of the feet and ankles is normal after a long day standing or sitting, such as waitressing or sitting at a desk all day. When swelling occurs for no apparent reason and the legs and feet become reddened, it can indicate a problem. Swelling of the lower extremities is referred to as edema and is due to retention water within the tissues. Certain metabolic diseases, injuries and infections can cause the feet and ankles to become red and swollen.
Injury
An injury to the foot or ankle can cause redness and pain to occur. In an injury, typically only one side of the body will be affected, but it is possible to injure both feet or ankles in a fall or car accident. According to the American Podiatric Medical Association, injuries such as fractures, strains, sprains and dislocations often occur. An ankle sprain can cause both the ankle and foot to become red and swollen, as can a fracture in the foot or ankle. A dislocation in the ankle or foot may cause the foot and ankle to become red and swollen. There will also be pain at the site of the injury. An injury should be assessed by a medical professional.
- An injury to the foot or ankle can cause redness and pain to occur.
- An ankle sprain can cause both the ankle and foot to become red and swollen, as can a fracture in the foot or ankle.
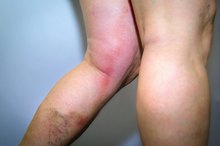
Cellulitis
Popliteal Aneurysm Symptoms
Learn More
Cellulitis is a serious bacterial infection of the skin. According to MayoClinic.com, cellulitis causes the skin to become red and swollen 1. It most commonly affects the legs, ankles and feet. Cellulitis occurs when bacteria invade through an opening or cut in the skin. The bacteria can also enter the skin via an insect or spider bite. The symptoms of cellulitis include red, swollen skin; pain and tenderness; and increased warmth in the affected area, along with a fever. Cellulitis that is spreading or occurs along with a fever requires evaluation by a physician immediately.
- Cellulitis is a serious bacterial infection of the skin.
- The bacteria can also enter the skin via an insect or spider bite.
Blood Clot
According to the Texas Heart Institute, about 6 million Americans have a blot clot, or thrombus, in a vein at any given time. Blood clots are caused by reduced blood flow, which allows a clot to form. Injury to a vein or physical inactivity can also cause a blood clot. The symptoms of a blood clot that occurs in the calf or foot includes redness and swelling, tenderness, warmth and pain at the site of the clot. A blood clot is a serious medical situation requiring immediate treatment and anti-coagulant medication.
- According to the Texas Heart Institute, about 6 million Americans have a blot clot, or thrombus, in a vein at any given time.
- Injury to a vein or physical inactivity can also cause a blood clot.
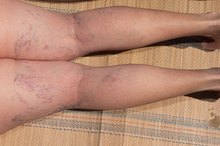
Venous Insufficiency
How to Get Rid of a Bruise From Cellulitis
Learn More
Venous insufficiency is condition that causes impairment of blood flow through the veins, according to the Cleveland Clinic 3. Varicose veins are one primary cause of venous insufficiency and are caused by damaged valves in the veins allowing backflow of blood 3. The blood tends to pool in the ankles and feet, allowing protein matter to leak into surrounding tissues, causing swelling. Over time, the skin on the ankles and feet can become reddened. Other symptoms include developing sores or ulcers that are slow to heal, prominent veins along with aching, cramping and weakness. The treatment for venous insufficiency includes wearing compression stockings to aid the blood flow returning to the heart 3.
Related Articles
References
- MayoClinic.com: Cellulitis
- Texas Heart Institute: Peripheral Vascular Disease
- Cleveland Clinic: Venous Insufficiency
- Boisseau, M. (2018). Chronic venous disease and the genetic influence - Servier - Phlebolymphology.
- Chaer, R. (2017). Vascular Disease in Older Adults. Cham: Springer, p.98.
- Cleveland Clinic. 2018. Chronic Venous Insufficiency (CVI) Treatment Options.
- Goldstein, E. and Weingarten, M. (2001). State-of-the-Art Treatment of Chronic Venous Disease. Clinical Infectious Diseases, 32(6), pp.949-954. DOI: 10.1086/319360.
- Vascularcures.org. (2018). Chronic Venous Insufficiency.
Writer Bio
Kathryn Meininger began writing and publishing poetry in 1967. She was co-founder and editor of the professional magazine "Footsteps" and began writing articles online in 2010. She earned a Doctor of Podiatric Medicine from Temple University School of Podiatric Medicine and a Bachelor of Arts in biology from William Paterson University.