The term “surrogate father” has at least three different meanings. One must surmise the particular meaning based on the context of the use of the term. The uses of “surrogate father” can be quite different and are virtually opposite in meaning.
Surrogate Father as Substitute Father
The most common use of "surrogate father" refers to a man who is not the biological, adoptive or step father, but who serves as a father figure. In this use of the term, the biological father is absent from the child’s life and the child becomes attached to the surrogate father. The surrogate father might be an older sibling, uncle, romantic partner to the mother, family friend or some other male figure who provides some measure of childcare, love, guidance, discipline, financial support or paternalistic companionship.
Importance of Surrogate Fathers
How Is Sperm Collected?
Learn More
Surrogate fathers have become increasingly important in modern culture. The breakdown of the nuclear family and the ever-increasing number of homes in which the biological father is absent has stressed children and families. According to a wide body of research, including research summarized by the National Fatherhood Initiative, children in homes with absent fathers suffer a variety of consequences, including financial distress, poor school performance, low esteem, behavior problems and greater risk for depression and other psychiatric problems. Surrogate fathers often step in and fulfill the father role. In one study reported by the American Sociological Association, more than a fifth of the children in a sample of urban families had a surrogate father involved in their lives. In this study, many of the children and mothers thought of the surrogate father as more important in the child’s life than the biological father.
- Surrogate fathers have become increasingly important in modern culture.
- In one study reported by the American Sociological Association, more than a fifth of the children in a sample of urban families had a surrogate father involved in their lives.
Legal Rights of Surrogate Fathers
Surrogate fathers may be important to children and mothers, but they have few legal rights. A surrogate father’s contributions to the child’s welfare do not grant him custody or visitation rights. He can potentially be denied contact with the child if the mother decides to cut the surrogate father off, or if something happens where the child’s custody changes, such as if the mother dies or goes to jail.
- Surrogate fathers may be important to children and mothers, but they have few legal rights.
- He can potentially be denied contact with the child if the mother decides to cut the surrogate father off, or if something happens where the child’s custody changes, such as if the mother dies or goes to jail.
Surrogate Father as Sperm Donor
Signs That Your Boyfriend Is Impotent
Learn More
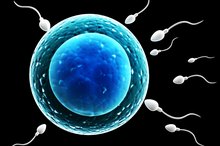
A second use of the term "surrogate father" describes a man who donates his sperm to a woman who wants to become pregnant when she does not have a male partner or her partner is infertile. The process of fertilization is done with the help of a fertility doctor. The mother-to-be can arrange for a person she knows to donate the sperm, or she can use the services of a clinic. When a sperm clinic is used, women can review information about the surrogate father, but the process is anonymous, and neither mother nor surrogate father have any direct contact. The surrogate father signs legal forms surrendering all rights to his sperm and any progeny that are created using it. Likewise, when the mother arranges for someone she knows to donate sperm, the surrogate father typically has no role in child rearing.
- A second use of the term "surrogate father" describes a man who donates his sperm to a woman who wants to become pregnant when she does not have a male partner or her partner is infertile.
- When a sperm clinic is used, women can review information about the surrogate father, but the process is anonymous, and neither mother nor surrogate father have any direct contact.
Fathering a Child Through Surrogacy
A third, less common use of the term "surrogate father" refers to a man who becomes a father by using a surrogate mother. If a man wishes to become a father but doesn’t have a partner, or his partner is infertile, he can find a woman who becomes an egg donor and bears the child. The child is surrendered at birth to the man. The surrogate father can find his own surrogate mother or can work through an agency that keeps the identity of the surrogate mother anonymous. Legal, financial and medical issues are usually handled by an agency that specializes in surrogacy.
- A third, less common use of the term "surrogate father" refers to a man who becomes a father by using a surrogate mother.
- The surrogate father can find his own surrogate mother or can work through an agency that keeps the identity of the surrogate mother anonymous.
Related Articles
Writer Bio
Jon Williams is a clinical psychologist and freelance writer. He has performed, presented and published research on a variety of psychological and physical health issues.