**The appendix is a small, nonessential organ attached to the large intestine near its connection to the small intestine.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
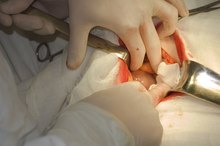
** When the appendix becomes inflamed or infected, it is usually removed.
Surgical removal of the appendix, known as an appendectomy, can be performed with an open procedure or using laparoscopic instruments.
Risks and side effects vary depending on the type of procedure, whether the appendix has ruptured, and other factors. Most side effects are mild and temporary, although serious complications sometimes occur.
Abdominal Pain and Discomfort
**Abdominal pain after an appendectomy is expected, but the severity varies among individuals.
** Postoperative pain typically decreases over time, and surgeons routinely prescribe pain medication as needed. Holding a pillow against your stomach when coughing or getting up can help minimize your pain with these activities.
Abdominal discomfort due to bloating is also common after a laparoscopic appendectomy. It occurs because gas is pumped into the abdomen during the procedure to enable the surgeon to maneuver the instruments and see your organs clearly.
This gas can also sometimes cause referred shoulder pain. Gas-related side effects are short-lived, as the gas dissipates in the first 24 to 48 hours after a laparoscopic procedure.
- Abdominal pain after an appendectomy is expected, but the severity varies among individuals.
- Gas-related side effects are short-lived, as the gas dissipates in the first 24 to 48 hours after a laparoscopic procedure.
Bowel Issues
Post Operative Complications of Abdominal-Hernia Surgery
Learn More
Since an appendectomy involves manipulation of the bowel, you might experience diarrhea for a few days after the procedure. Constipation can also occur, primarily due to narcotic pain medicines that may be prescribed. Ileus -- temporary lack of normal bowel contractions -- can occur with any type of abdominal surgery. Symptoms include nausea, vomiting and abdominal distention. This condition normally resolves on its own within a few days, although it may prolong your hospital stay. Less commonly, a temporary bowel obstruction can occur due to bowel swelling near the site where the appendix was removed. This situation also typically resolves with a few days of appropriate treatment in the hospital. Scar tissue formation after an appendectomy can increase the risk of a bowel obstruction years after the procedure, although this is a rare complication 1.
- Since an appendectomy involves manipulation of the bowel, you might experience diarrhea for a few days after the procedure.
- Ileus -- temporary lack of normal bowel contractions -- can occur with any type of abdominal surgery.
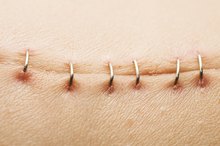
Wound Infection
A surgical wound infection is the most common, serious complication after an appendectomy, according to the American College of Surgeons 5.
These infections are more common with an open appendectomy compared to a laparoscopic procedure 7. People who smoke may be an increased risk for postoperative wound infections.
Rupture of the appendix before surgery also increases the risk for an infection at the site of the surgical incision 4. Most surgical wound infections are treated successfully with antibiotics, but other treatment may be needed.
- A surgical wound infection is the most common, serious complication after an appendectomy, according to the American College of Surgeons 5.
- These infections are more common with an open appendectomy compared to a laparoscopic procedure 7.
Abdominal Infection
Side Effects of Tubalectomy
Learn More
An emergency appendectomy is performed with suspected appendicitis because if the appendix ruptures, bowel bacteria escapes into and infects the abdominal cavity. This infection, known as peritonitis, is a serious complication of appendicitis. However, peritonitis can also develop as a rare complication of appendix removal surgery.
An unnoticed, accidental nick of the bowel during surgery is usually the culprit when peritonitis develops after an appendectomy 1. Formation of an abscess -- a pocket of infection -- in the abdomen near the site where the appendix was removed is another possible, rare complication after an appendectomy. Development of an abscess in the abdomen after appendix removal may require a second surgery to drain the abscess.
- An emergency appendectomy is performed with suspected appendicitis because if the appendix ruptures, bowel bacteria escapes into and infects the abdominal cavity.
- An unnoticed, accidental nick of the bowel during surgery is usually the culprit when peritonitis develops after an appendectomy 1.
General Side Effects of Surgery and Anesthesia
Certain side effects are possible with any abdominal surgical procedure, including an appendectomy. These potential but uncommon complications include: -- pneumonia -- blood clot formation -- development of a hernia -- heart attack during or after surgery -- reaction to anesthesia -- excessive bleeding
Rarely, serious complication can lead to death.
Some complications, length of stay in the hospital and number of deaths are lower with a laparoscopic appendectomy compared to an open procedure, according to an analysis of the medical research published in October 2010 by the "Cochrane Database of Systematic Reviews." However, there are situations in which an open appendectomy is preferable to a laparoscopic procedure 37.
- Certain side effects are possible with any abdominal surgical procedure, including an appendectomy.
- However, there are situations in which an open appendectomy is preferable to a laparoscopic procedure 3.
Warnings and Precautions
Most people undergoing an appendectomy experience only mild, short-term side effects and return to their regular activities within 2 to 4 weeks. However, serious side effects are possible, so it's important to watch for warning signs. Your doctor will give you specific postoperative instructions, but the American College of Surgeons recommends contacting your doctor if you experience: -- persistent, worsening or severe abdominal pain -- repeated vomiting -- a fever higher than 101 F -- watery diarrhea or no bowel movements for 3 days -- swelling, redness, bleeding or foul-smelling drainage from your surgical incisio 5n
Reviewed and revised by: Tina M. St. John, M.D.
Related Articles
References
- Annals of Surgery: Bowel Obstruction Following Appendectomy: What is the True Incidence?
- Merck Manual Professional Version: Ileus (Paralytic Ileus; Adynamic Ileus; Paresis)
- Cochrane Database of Systematic Reviews: Laparoscopic Versus Open Surgery for Suspected Appendicitis
- Annals of Surgery: Risk Factors for Adverse Outcomes After the Surgical Treatment of Appendicitis in Adults
- American College of Surgeons: Appendectomy
- Journal of Medicine and Life: Laparoscopic Surgery Complications: Postoperative Peritonitis
- General Surgery: Principles and International Practice, 2nd Edition; Kirby I. Bland, et al.
- Essentials of General Surgery, 5th Edition; Peter F. Lawrence
- Complications in Surgery and Trauma, 2nd Edition; Stephen M. Cohn and Matthew O. Dolich
- U.S. National Library of Medicine: MelinePlus. Appendicitis. Updated March 18, 2019.
- SAGES: Society of American Gastrointestinal and Endoscopic Surgeons. Appendix removal (appendectomy) surgery patient information from SAGES.
- SAGES: Society of American Gastrointestinal and Endoscopic Surgeons. Guidelines for laparoscopic appendectomy.
- U.S. National Library of Medicine: MedlinePlus. Appendectomy. Updated April 9, 2020.
- American College of Surgeons. Appendectomy. Updated 2017.
- John Hopkins Medicine. Appendectomy.
- Scott A, Shekherdimian S, Rouch JD, et al. Same-day discharge in laparoscopic acute non-perforated appendectomy. J Am Coll Surg. 2017;224(1):43-48. doi:10.1016/j.jamcollsurg.2016.10.026
- Mayo Clinic. Pain medications after surgery. Updated February 22, 2020.
- U.S. National Library of Medicine: MedlinePlus. Acetaminophen. Updated April 20, 2020
- Rasmussen T, Fonnes S, Rosenberg J. Long-Term Complications of Appendectomy: A Systematic Review. Scand J Surg. 2018;107(3):189-196. doi:10.1177/1457496918772379
Writer Bio
Marcy Brinkley has been writing professionally since 2007. Her work has appeared in "Chicken Soup for the Soul," "Texas Health Law Reporter" and the "State Bar of Texas Health Law Section Report." Her degrees include a Bachelor of Science in Nursing; a Master of Business Administration; and a Doctor of Jurisprudence.