What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
CPR Vs. Rescue Breathing
Cardiopulmonary resuscitation and rescue breathing are skills used when a person has fallen victim to sudden cardiac or respiratory arrest. Both of these situations pose an immediate threat to life. While effective CPR is known to double or triple a person's chances for surviving sudden cardiac arrest, less than one-third of people who arrest outside of the hospital receive bystander CPR.
Rescue breathing
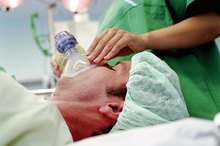
Rescue breathing is a skill performed for a victim who is not breathing at all, or whose breaths are too slow or irregular to be effective. In rescue breathing, breaths are delivered to the victim by pinching the nose shut and breathing into the victim's mouth. This is done to deliver oxygen to the victim to help their brain and vital organs survive. Masks and other barrier devices are available to decrease the risk disease transmission when giving rescue breaths.
- Rescue breathing is a skill performed for a victim who is not breathing at all, or whose breaths are too slow or irregular to be effective.
- In rescue breathing, breaths are delivered to the victim by pinching the nose shut and breathing into the victim's mouth.
Chest Compressions
How to Perform CPR on a Person With a Pacemaker
Learn More
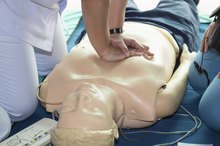
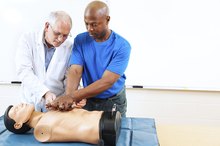
When a person suffers sudden cardiac arrest, death is imminent unless he receives help immediately. In CPR, rescue breathing is combined with chest compressions to send oxygen-containing blood to the brain and vital organs for a person who is not breathing and whose heart is not beating.The rescuer applies chest compressions by pushing down on the victim's breastbone, between the nipples This action pushes down on the heart, forcing blood to circulate. Cycles of rescue breaths and chest compressions continue until medical help arrives.
Benefits
Sudden cardiac arrest can happen to a person of any age. Friends, family or even strangers trained to respond can increase the victim's chances for survival. Effective rescue breathing allows the victim who is not breathing to receive the oxygen that is necessary to sustain life. Chest compressions push blood to the brain and vital organs. In addition to calling for emergency medical help, bystander CPR increases the victim's chances for surviving the event.
- Sudden cardiac arrest can happen to a person of any age.
- Friends, family or even strangers trained to respond can increase the victim's chances for survival.
Compression-Only CPR
Conditions That Must Exist Before Using CPR
Learn More
The American Heart Association issued a statement in 2008 that the use of compression-only CPR could be an effective means of providing CPR to an adult victim of a sudden, witnessed, cardiac arrest in the community setting 124. In compression-only CPR, the rescuer performs only chest compressions, without pausing to deliver rescue breaths The American Heart Association acknowledged that the fear of performing mouth-to-mouth breathing is a significant deterrent to bystander response, and that performing compression-only CPR was more helpful than doing no CPR at all 124.
Learning More
CPR skills, including rescue breathing, can mean the difference between life and death in an emergency. The American Red Cross and the American Heart Association offer classes in many communities 124. There are also online training opportunities, and the CPR Anytime kit is available from the American Heart Association 124. CPR Anytime includes a manikin and video to allow people to learn and practice the skills of CPR right in their own home.
Related Articles
References
- American Heart Association: Hand-Only (Compression-Only) CPR
- American Heart Association: Agonal Breathing/Gasping
- MedlinePlus: Breathing - slowed or stopped
- American Heart Association: CPR Statistics
- Panchal AR, Berg KM, Kudenchuk PJ, et al. 2018 American Heart Association Focused Update on Advanced Cardiovascular Life Support Use of Antiarrhythmic Drugs During and Immediately After Cardiac Arrest: An Update to the American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2018;138:e740-e749. doi:10.1161/CIR.0000000000000613
- Aufderheide TP, Frascone RP, Wayne MA, et al. Standard cardiopulmonary resuscitation versus active compression-decompression cardiopulmonary resuscitation with augmentation of negative intrathoracic pressure for out-of-hospital cardiac arrest: a randomised trial. Lancet. 2011;377(9762):301-11. doi:10.1016/S0140-6736(10)62103-4
Resources
Writer Bio
Kathy Dropeski began writing for various websites since 2010. She has been published in the American Association of Diabetes Educator's "AADE in Practice" and has produced numerous patient teaching materials and local news articles. Dropeski obtained her bachelor's degree in nursing from Concordia University. She has been a registered nurse since 1995 and a certified diabetes educator since 2005.