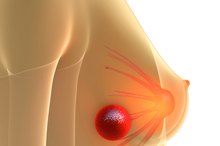
Symptoms of Breast Cancer Metastasizing to the Shoulder
Breast cancer typically develops when glandular tissue of the breast becomes mutated. The cells begin to divide rapidly, giving rise to unlimited daughter cells, evading cellular death and accumulating genetic mutations that help further drive cancer development. Over time, breast cancer cells gain the ability to invade other cells and tissues throughout the body. In some cases, breast cancer spreads to tissues within and around the shoulder, leading to a number of symptoms.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Pain
The development of joint pain is a common symptom of breast cancer metastasizing to the shoulder. As the breast cancer cells colonize tissues in the shoulder, they attack neighboring healthy cells and cause tissue damage that can lead to pain. A study published in "Current Oncology" in 2006 indicates that breast cancer metastasis can lead to the development of cancerous lesions of the humerus, the upper arm bone 1. As the cancer forms growth on the head of the humerus, where the arm meets the shoulder joint, the tumors can interfere with normal joint functioning, leading to pain when moving the shoulder. Breast cancer patients experiencing unexplained shoulder pain should seek medical attention to assess the possibility of breast cancer to the shoulder joint.
- The development of joint pain is a common symptom of breast cancer metastasizing to the shoulder.
- A study published in "Current Oncology" in 2006 indicates that breast cancer metastasis can lead to the development of cancerous lesions of the humerus, the upper arm bone 1.
Bone Fractures
Causes of Left Shoulder Blade Pain
Learn More
If breast cancer growth on the bones around the shoulder goes undetected, patients may become vulnerable to bone fractures. Many breast cancers form osteolytic lesions on bone tissue--they recruit cells that help break down healthy bone around the tumor, according to a study published in "Carcinogenesis" in 2009. As the cancer progresses, the progressive loss of bone tissue significantly weakens the bone, eventually leaving the patient vulnerable to bone fractures. The use of drug therapies can help slow the bone loss associated with breast cancer metastasis and help protect against bone injuries due to cancer growth.
- If breast cancer growth on the bones around the shoulder goes undetected, patients may become vulnerable to bone fractures.
- As the cancer progresses, the progressive loss of bone tissue significantly weakens the bone, eventually leaving the patient vulnerable to bone fractures.
Swollen Lymph Nodes
Another potential symptom of breast cancer metastasis to the shoulder is the development of enlarged lymph nodes. Lymph nodes, small structures that house immune system cells called lymphocytes, are found around the breasts and shoulder, under the arm and throughout the body. Breast cancer cells can begin to colonize lymph nodes, leading to an enlargement and matting of the nodes. If breast cancer spreads to lymph nodes in the shoulder, patients may notice a lump under the arm corresponding to clusters of enlarged lymph nodes. Over time, cancer cells in the lymph nodes can enter the lymph vessels and metastasize, colonizing tissues in the shoulder or other distant tissues throughout the body. Although other medical conditions, such as infections, can lead to swollen lymph nodes, unexplained lumps in the arm pit or shoulder should be examined for the presence of cancer.
- Another potential symptom of breast cancer metastasis to the shoulder is the development of enlarged lymph nodes.
- If breast cancer spreads to lymph nodes in the shoulder, patients may notice a lump under the arm corresponding to clusters of enlarged lymph nodes.
Related Articles
References
- Current Oncology: Solitary bone metastasis beneath the shoulder shield: coincidence or cause?
- Carcinogenesis: Selenium modifies the osteoblast inflammatory stress response to bone metastatic breast cancer
- American Cancer Society. Understanding advanced cancer, metastatic cancer, and bone metastasis. Updated December 15, 2016.
- Redig AJ, McAllister SS. Breast cancer as a systemic disease: a view of metastasis. J Intern Med. 2013;274(2):113–126. doi:10.1111/joim.12084
- American Cancer Society. What is cancer recurrence? Updated February 12, 2016.
- American Society of Clinical Oncology. Breast cancer—metastatic: Risk factors. Updated April, 2019.
- Giles AJ, Reid CM, Evans JD, et al. Activation of hematopoietic stem/progenitor cells promotes immunosuppression within the pre-metastatic niche. Cancer Res. 2016;76(6):1335-47. doi:10.1158/0008-5472.CAN-15-0204
- Shukla A, Alsarraj J, Hunter K. Understanding susceptibility to breast cancer metastasis: the genetic approach. Breast Cancer Manag. 2014;3(2):165-172. doi:10.2217/bmt.14.1
- Metastatic Breast Cancer Research (MBCR). What is Metastatic Breast Cancer? Updated October 13,2019.
- Iqbal N, Iqbal N. Human epidermal growth factor receptor 2 (HER2) in cancers: overexpression and therapeutic implications. Mol Biol Int. 2014;2014:852748. doi:10.1155/2014/852748
- Garcia-closas M, Chanock S. Genetic susceptibility loci for breast cancer by estrogen receptor status. Clin Cancer Res. 2008;14(24):8000-9. doi:10.1158/1078-0432.CCR-08-0975
- American Society of Clinical Oncology. Breast cancer: Risk factors and prevention. Updated July, 2019.
- Susan G. Koman. Getting the support you need. Updated June 2, 2017.
Writer Bio
Sylvie Tremblay holds a Master of Science in molecular and cellular biology and has years of experience as a cancer researcher and neuroscientist. Based in Ontario, Canada, Tremblay is an experienced journalist and blogger specializing in nutrition, fitness, lifestyle, health and biotechnology, as well as real estate, agriculture and clean tech.