What Is Normal Blood Sugar in People Over 60?
Glucose, derived from foods and body stores, is a main source of energy to the body. Some health conditions, most notably prediabetes and diabetes, are characterized by elevated levels of glucose — or sugar — in the blood, and blood sugar tests are used to screen for, and to monitor these disorders.
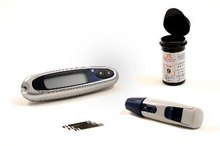
Blood sugar levels can also be checked at home, using a glucose meter or other devices. Normal ranges for laboratory blood sugar tests are the same for adults of all ages. However, recommended targets for home testing will sometimes be different for older adults.
Fasting Blood Glucose
When blood work is completed in a laboratory, blood sugar is often tested after an 8 to 12-hour fast. In this setting, normal fasting blood sugar is defined as less than 100 mg/dL, and as low as 60 to 70 — depending on the specific laboratory's reference range.
According to the American Diabetes Association's (ADA) 2018 clinical practice guidelines, fasting blood sugars between 100 to 125 are classified as prediabetes, and fasting readings above 125 fall into the diabetes range 1. These numbers are the same for all adults, including those over the age of 60.
- When blood work is completed in a laboratory, blood sugar is often tested after an 8 to 12-hour fast.
- In this setting, normal fasting blood sugar is defined as less than 100 mg/dL, and as low as 60 to 70 — depending on the specific laboratory's reference range.
Nonfasting Blood Glucose
What Are the Normal A1c Levels for Children?
Learn More
Blood sugars checked outside of a fasting state are commonly called random tests. Normal random blood sugar is not clearly defined, but a result above 200 is suggestive of diabetes.
Another test used for diagnosis is the oral glucose tolerance test (OGTT), which involves checking a fasting blood sugar, drinking a carbohydrate-containing liquid, then having the blood sugar checked again in 2 hours. A normal OGTT result falls below 140. The prediabetes range for the OGTT result is 140 to 199, and diabetes is considered when this result is above 200. These normal and diagnostic ranges apply to adults of all ages.
- Blood sugars checked outside of a fasting state are commonly called random tests.
- The prediabetes range for the OGTT result is 140 to 199, and diabetes is considered when this result is above 200.
Home Glucose Monitoring
If you are diagnosed with diabetes, your doctor or diabetes educator may recommend you start self monitoring your blood glucose (SMBG), which involves testing your own sugars using a glucose meter. Alternatively, your doctor may recommend a continuous glucose monitor (CGM), which senses blood glucose on a continual basis.
In these situations, you will be provided with target blood sugar ranges — which will be different, and a bit higher — compared to normal, nondiabetic blood sugars. According to the ADA, reasonable SMBG targets for most adults are 80 to 130 before meals and, when testing 2 hours after meals, below 180. However, your healthcare team may provide you with slightly different targets.
- If you are diagnosed with diabetes, your doctor or diabetes educator may recommend you start self monitoring your blood glucose (SMBG), which involves testing your own sugars using a glucose meter.
- In these situations, you will be provided with target blood sugar ranges — which will be different, and a bit higher — compared to normal, nondiabetic blood sugars.
Specific Advice for Older Adults
Normal Blood Sugar Range in Adults
Learn More
Many older adults with diabetes who are otherwise healthy and independent can try to achieve the same SMBG targets as their younger counterparts.
However, in some people, aiming for these near-normal blood sugars may increase the risk of hypoglycemia, or low blood sugar — a side effect of insulin or certain diabetes pills which can increase the risk of falls, confusion or accidents.
To avoid hypoglycemia, ADA recommends that physicians individualize — and relax — blood sugar targets in older adults who have multiple chronic illnesses, cognitive impairment or those who rely on others for daily care.
Warnings
If you have prediabetes or diabetes, your doctor will review a management plan tailored for you. Lifestyle therapy, including a healthy diet, weight management and exercise, is the cornerstone of managing these conditions. Medications may also be advised.
Blood sugar monitoring helps you understand how your blood sugars compare to your targets, and allows you to provide your doctor with specific data on your progress. Ask your doctor for a referral to a prediabetes or diabetes education program, so you can learn how to manage your condition, and also for a referral to a dietitian, for an individualized nutrition plan.
Reviewed by Kay Peck, MPH RD
- If you have prediabetes or diabetes, your doctor will review a management plan tailored for you.
- Ask your doctor for a referral to a prediabetes or diabetes education program, so you can learn how to manage your condition, and also for a referral to a dietitian, for an individualized nutrition plan.
Related Articles
References
- American Diabetes Association: Diagnosing Diabetes and Learning About Prediabetes
- Diabetes Care: Glycemic Targets: Standards of Medical Care in Diabetes—2018
- Diabetes Care: Classification and Diagnosis of Diabetes: Standards of Medical Care in Diabetes—20
- Diabetes Care: Older Adults: Standards of Medical Care in Diabetes—2018
- Centers for Disease Control and Prevention. National diabetes statistics report, 2020. Last reviewed February 11, 2020.
- Centers for Disease Control and Prevention. Diabetes symptoms. Last reviewed March 24, 2020.
- American Diabetes Association. Skin complications. 2019.
- American Diabetes Association. 2. Classification and diagnosis of diabetes: Standards of medical care in diabetes-2020. Diabetes Care. 2020;43(Suppl 1):S14-S31. doi:10.2337/dc20-S002
- National Institutes of Health: National Institute of Diabetes and Digestive and Kidney Diseases. Diabetes tests & diagnosis. 2016.
- Evert AB, Dennison M, Gardner CD, et al. Nutrition therapy for adults with diabetes or prediabetes: A consensus report. Diabetes Care. 2019;42(5):731-754. doi:10.2337/dci19-0014
- National Institutes of Health: National Institute of Diabetes and Digestive and Kidney Diseases. Symptoms and causes of diabetes. 2016.
- Roberts CK, Hevener AL, Barnard RJ. Metabolic syndrome and insulin resistance: underlying causes and modification by exercise training. Compr Physiol. 2013;3(1):1–58. doi:10.1002/cphy.c110062
- Hage M, Zantout MS, and Azar ST. Thyroid disorders and diabetes mellitus. Journal of Thyroid Research. 2011. Article ID 439463. 10.4061/2011/439463.
- American Diabetes Association. The Big Picture: Checking Your Blood Glucose
- American Diabetes Association. 6. Glycemic Targets: Standards of Medical Care in Diabetes-2020. Diabetes Care. 2020;43(Suppl 1):S66-S76. doi:10.2337/dc20-S006
- Centers for Disease Control and Prevention. Diabetes. Getting Tested
- American Diabetes Association. 2. Classification and Diagnosis of Diabetes: Standards of Medical Care in Diabetes-2020. Diabetes Care. 2020;43(Suppl 1):S14-S31. doi:10.2337/dc20-S002
- American Diabetes Association. 2. Classification and Diagnosis of Diabetes: Diabetes Care. 2018;41(Suppl 1):S13-S27. doi:10.2337/dc18-S002
- American Diabetes Association. Understanding A1C
- Joslin Diabetes Center. Home Blood Glucose (Sugar) Monitoring, Hemoglobin A1c Testing, and Fructosamine Tests
- Johns Hopkins Medicine. Alternative markers of glycemia: fructosamine, glycated albumin, 1,5-AG. January 2014.
- American Diabetes Association. 14. Management of Diabetes in Pregnancy: Standards of Medical Care in Diabetes-2020. Diabetes Care. 2020;43(Suppl 1):S183-S192. doi:10.2337/dc20-S014
- American Diabetes Association. 13. Children and Adolescents: Standards of Medical Care in Diabetes-2020. Diabetes Care. 2020;43(Suppl 1):S163-S182. doi:10.2337/dc20-S013
- American Diabetes Association. Standards of Medical Care in Diabetes-2020. Diabetes Care. 2020;43(Suppl 1).
- Ayyappan S, Philips S, Kumar CK, Vaithiyanandane V, Sasikala C. Serum fructosamine a better indicator than glycated hemoglobin for monitoring gestational diabetes mellitus. Journal of Pharmacy & Bioallied Sciences. 2015;7(Suppl 1):S32-S34. doi:10.4103/0975-7406.155786.
Writer Bio
Carol Ochs is an award-winning writer in the Washington, D.C. area. During 17 years with The Associated Press she covered health, medical and sports stories as a writer, editor and producer. She has written for the health section of "The Washington Post," a Fairfax County stewardship publication and a biopharmaceutical newsletter. Ochs has a Bachelor of Science in journalism from Ohio University, Athens.