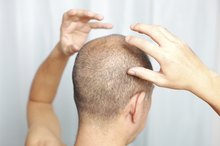
Alopecia areata is a condition in which an autoimmune response causes hair loss. About 2 percent of Americans have some form of the disease, according to the National Alopecia Areata Foundation 1. Any part of the body with hair can be affected, but eyelashes and eyebrows typically only fall out in people with severe cases, according to a study published in the Dermatology Online Journal 2. Furthermore, cases of alopecia involving only the eyelashes are extremely rare, the journal reports 2.
Onset
In the typical progression of alopecia, hair loss becomes noticeable on the scalp, then begins affecting the eyelashes and other parts of the body. Alopecia strictly affecting the eyelashes is a rarely seen presentation of the condition, according to Dermatology Online Journal 2. In these cases, the condition rarely spreads to other hair-bearing parts of the body, such as the scalp.
Symptoms
Scalp Conditions That Cause Hair Loss
Learn More
With all forms of alopecia, hair loss generally occurs gradually and may not be immediately noticeable. Over time, you may notice coin-sized bald patches on the scalp. The hair loss typically produces no other symptoms, although you may experience an itching sensation on the scalp before hair begins to fall out. In patients whose eyelashes are extensively involved, hair loss often occurs in clumps on both the upper and lower eyelids.
- With all forms of alopecia, hair loss generally occurs gradually and may not be immediately noticeable.
- In patients whose eyelashes are extensively involved, hair loss often occurs in clumps on both the upper and lower eyelids.
Cause
Alopecia areata occurs because the body's immune system attacks the hair follicles, according to the National Alopecia Areata Foundation 1. Researchers have not determined why the immune system begins attacking hair follicles, but both genetics and environmental factors are believed to play a role. People of all ages and ethnicities develop alopecia areata, and it most commonly develops in young adults and children. In about 20 percent of cases, a person with the condition also has a family member who has alopecia, the American Academy of Dermatology reports.
- Alopecia areata occurs because the body's immune system attacks the hair follicles, according to the National Alopecia Areata Foundation 1.
Treatment
Eyelash Growth Cycle
Learn More
There is no cure for alopecia areata, but treatments can be used to encourage hair growth. One such option is corticosteroid injections into the site where hair loss has occurred. You will generally notice new hair growth about a month after treatment starts, the American Academy of Dermatology reports. In some cases, the corticosteroids can be taken orally or be applied topically to the area where hair has fallen out. When much of a person's hair is involved, more invasive treatments such as hair transplants can be considered. Wigs and hairpieces also are available for people who experience drastic hair loss.
- There is no cure for alopecia areata, but treatments can be used to encourage hair growth.
- One such option is corticosteroid injections into the site where hair loss has occurred.
Prognosis
In many cases, hair that falls out from alopecia areata -- including eyelashes, eyebrows and facial hair -- will grow back. However, many people with the condition will continue to experience bouts of hair loss throughout the course of their lives, according to the American Academy of Dermatology. Some people continue to experience patchy hair loss or even extensive or total hair loss continuously. The condition itself is not a sign of a more serious illness, but people with alopecia areata are more likely to develop some other autoimmune conditions, including vitiligo and Hashimoto's disease.
- In many cases, hair that falls out from alopecia areata -- including eyelashes, eyebrows and facial hair -- will grow back.
- However, many people with the condition will continue to experience bouts of hair loss throughout the course of their lives, according to the American Academy of Dermatology.
Related Articles
References
- National Alopecia Areata Foundation: About Alopecia Areata
- Dermatology Online Journal, Volume 10, Number 2: Alopecia of the Eyelashes: A Subset of Alopecia Areata
- University of Maryland Medical Center: Alopecia Areata
- Alessandrini A, Starace M, Bruni F et al. Alopecia areata incognita and diffuse alopecia areata: clinical, trichoscopic, histopathological, and therapeutic features of a 5-year study. Dermatol Pract Concept. 2019:272-277. doi:10.5826/dpc.0904a05
- El-Taweel A, El-Esawy F, Abdel-Salam O. Different trichoscopic features of tinea capitis and alopecia areata in pediatric patients. Dermatol Res Pract. 2014;2014:1-6. doi:10.1155/2014/848763
- Pratt CH, King LE Jr, Messenger AG, Christiano AM, Sundberg JP. Alopecia areata. Nat Rev Dis Primers. 2017 Mar 16;3:17011. doi:10.1038/nrdp.2017.11
- Wang S, Ratnaparkhi R, Piliang M, Bergfeld WF. Role of family history in patchy alopecia areata. Dermatol Online J. 2018 Oct 15;24(10). pii: 13030/qt0n19r7ps.
- Thompson JM, Park MK, Qureshi AA, Cho E. Race and Alopecia Areata amongst US Women. J Investig Dermatol Symp Proc. 2018;19(1):S47-S50. doi:10.1016/j.jisp.2017.10.007
- Putterman E, Castelo-soccio L. Seasonal patterns in alopecia areata, totalis, and universalis. J Am Acad Dermatol. 2018;79(5):974-975. doi:10.1016/j.jaad.2018.06.029
- Hordinsky MK. Alopecia areata: The clinical situation. J Investig Dermatol Symp Proc. 2018 Jan;19(1):S9-S11. doi:10.1016/j.jisp.2017.10.015
- Wang EHC, Sallee BN, Tejeda CI, Christiano AM. Montagna Symposium 2017 - Janus Kinase inhibitors for treatment of alopecia areata. J Invest Dermatol. 2018 Sep; 138(9):1911–1916. doi:10.1016/j.jid.2018.05.027
- Peloquin L, Castelo-Soccio L. Alopecia areata: An update on treatment options for children. Paediatr Drugs. 2017 Oct;19(5):411-422. doi:10.1007/s40272-017-0239-z
- Strazzulla LC, Wang EHC, Avila L, et al. Alopecia areata: Disease characteristics, clinical evaluation, and new perspectives on pathogenesis. J Am Acad Dermatol. 2018 Jan;78(1):1-12. doi:10.1016/j.jaad.2017.04.1141
- Strazzulla LC, Wang EHC, Avila L, et al. Alopecia areata: An appraisal of new treatment approaches and overview of current therapies. J Am Acad Dermatol. 2018 Jan;78(1):15-24. doi:10.1016/j.jaad.2017.04.1142
- Trüeb RM, Dias MFRG. Alopecia areata: Acomprehensive review of pathogenesis and management. Clin Rev Allergy Immunol. 2018 Feb;54(1):68-87. doi:10.1007/s12016-017-8620-9
Writer Bio
Anna Aronson began working as a journalist in 2000 and spent six years at suburban Chicago newspapers before pursuing freelance work. She enjoys writing about health care topics, in particular obstetrics, pediatrics and nutrition. She received a Bachelor of Arts in journalism from Eastern Illinois University and is now studying for a Master of Science in medicine degree to become a physician's assistant.