What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
- National LIbrary of Medicine: Scars
- National Institutes of Health: Skin Scarring
- National Institutes of Health: Skin Scarring
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
Healing Stages of Scars
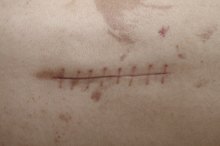
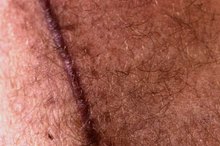
Scars are the result of the healing process. Collagen forms beneath the skin as a part of the process of wound healing. Scars are formed from wounds, burns, surgeries, accidents, stretch marks and skin diseases. Scars heal differently based upon the type of wound and individual factors that determine the size and look of the scar. Scars heal in three phases: the inflammatory stage, the proliferative stage and the remodeling stage.
Inflammatory Stage
The inflammatory stage is the first stage. It lasts only a few days. At this stage, the wound is red and inflamed. Bleeding stops and antibodies rush to the site of the wound to fight infection. As the body starts to heal, it produces new cells and healing tissue. The increased blood flow is what causes the discoloration, according to the Free Medical Dictionary 4. Scabbing over of the wound is also part of the inflammatory stage. The scab serves as a protective covering on the wound while it heals.
- The inflammatory stage is the first stage.
- Scabbing over of the wound is also part of the inflammatory stage.
Proliferative Stage
Lotion to Remove Scars
Learn More
The proliferative stage lasts about three to four weeks. Skin-forming cells, called fibroblasts, proliferate at the site of the wound. These fibroblasts produce collagen. Collagen continues to form for up to two weeks, pulling the edges of the wound together. Tiny blood vessels and capillaries form to help heal the wound. The growth of collagen causes the wound to become thicker and redder in appearance.
An over-active healing process can cause extra production of collagen that builds up on the wound causing a raised, or keloid scar. Keloids can cause itchiness, redness, unusual sensations and even pain, according to the American Osteopathic College of Dermatology 2. Darker skinned people are more prone to keloids, but lighter skinned people can develop keloids also.
- The proliferative stage lasts about three to four weeks.
- Collagen continues to form for up to two weeks, pulling the edges of the wound together.
Remodeling Stage
In the remodeling stage, scars start to fade and thin out. This stage continues for a few weeks to a few years, according to the Cleft Palate Foundation. Over time, some scars fade to a thin white line and are barely noticeable.
Genetics play an important role in how a scar will heal. Some scars produce lighter, flatter scars, while others produce darker, thicker scars. Illnesses can slow the healing process and change how a wound heals. Certain vitamins help the body in the healing process, such as vitamin C and zinc. Other factors that affect how a scar will look include whether you smoke, skin quality and blood supply to the area.
- In the remodeling stage, scars start to fade and thin out.
- Illnesses can slow the healing process and change how a wound heals.
Related Articles
References
- National LIbrary of Medicine: Scars
- American Academy of Dermatology: What is a Scar
- National Institutes of Health: Skin Scarring
- The Free Dictionary: Medical Dictionary: Scars
- Fabbrocini, G, Annunziata, MC, D'Arco, V, et al. Acne scars: pathogenesis, classification and treatment. Dermatol Res Pract. 2010;2010:893080. doi:10.1155/2010/893080
- Kravvas G, Al-niaimi F. A systematic review of treatments for acne scarring. Part 1: Non-energy-based techniques. Scars Burn Heal. 2017;3:2059513117695312. doi:10.1177/2059513117695312
- Gozali MV, Zhou B. Effective treatments of atrophic acne scars. J Clin Aesthet Dermatol. 2015;8(5):33-40.
- Wollina U, Goldman A. Fillers for the improvement in acne scars. Clin Cosmet Investig Dermatol. 2015;8:493-9. doi:10.2147/CCID.S86478
- Kravvas G, Al-niaimi F. A systematic review of treatments for acne scarring. Part 2: Energy-based techniques. Scars Burn Heal. 2018;4:2059513118793420. doi:10.1177/2059513118793420
- Ogawa R. Keloid and hypertrophic scars are the result of chronic inflammation in the reticular dermis. Int J Mol Sci. 2017;18(3). doi:10.3390/ijms18030606
- Rabello FB, Souza CD, Farina júnior JA. Update on hypertrophic scar treatment. Clinics (Sao Paulo). 2014;69(8):565-73. doi:10.6061/clinics/2014(08)11
- França K, Keri J. Psychosocial impact of acne and postinflammatory hyperpigmentation. An Bras Dermatol. 2017;92(4):505-509. doi:10.1590/abd1806-4841.20175645
- Tosti, A, De Padova, MP, Beer, KR, eds. Acne Scars: Classification and Treatment. London: Informa UK Ltd.; 2010.
Writer Bio
Caroline Thompson is a professional photojournalist who has been working for print and online publications since 1999. Her work has appeared in the "Sacramento Bee," "People Magazine," "Newsweek" and other publications. She holds a Bachelor of Arts in photojournalism from California State University at Hayward and a personal trainer certification from the university's Health and Fitness Institute.