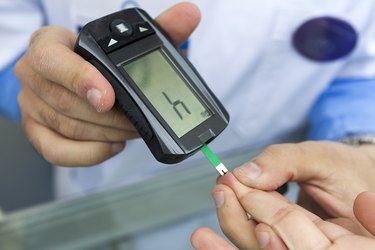
Eating big meals can cause your blood sugar levels to increase dramatically. If you are otherwise healthy, your body has a system to quickly usher the blood sugar out of your blood and into the cells where it belongs. However, if you have a condition like insulin resistance or diabetes, the consequences of big meals on blood sugar levels are more dire. Repeated overdoses on food set the stage for chronically elevated blood sugar levels, which can damage your organs.
What Happens When You Eat
Video of the Day

Your body is an incredible piece of machinery designed to take the energy and nutrients from your food and transform them for use by your body. When you have a meal, your digestive system breaks down the food. As you digest, some of that broken-down food becomes a simple sugar called glucose. Glucose is the most common carbohydrate and is a basic building block of other sugars and carbohydrates. Glucose next enters your bloodstream and that's partly why it's called blood sugar. It normally circulates in concentrations of 65 to 110 mg/mL, according to Elmhurst College's "Virtual Chembook." Your pancreas, sensing the increase in blood sugar after you've eaten, releases a hormone called insulin. Insulin shuttles glucose from your blood into your cells for energy and into your muscles and liver for storage. Some people, such as those who have diabetes, have trouble with insulin. In many cases, insulin doesn't work and blood sugar builds up in the bloodstream.
Video of the Day
Postprandial Blood Sugar
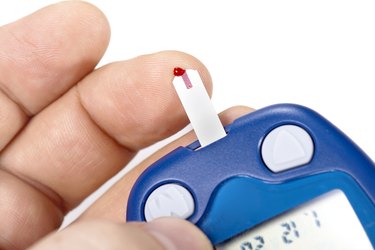
When your doctor measures your blood sugar, she will generally test you in two different states: your fasting state and your postprandial state. Postprandial means after a meal, and your fasting state refers to times when you haven't eaten and your digestion has been completed. When you eat, the time it takes for glucose to hit your bloodstream depends on a number of factors, such as how much of your meal was carbohydrates and how much of those carbohydrates were simple sugars like white bread, sugary drinks and desserts, what else you ate and how much you ate. Eating frequency also plays a role in your blood sugar level.
Big Meals and Blood Sugar

Your blood sugar response can start within 15 minutes for a meal full of simple carbs, and can linger for up to two hours. When you have an especially large meal, you can supply your body with more blood sugar than you need. A big, starchy meal can raise your blood sugar levels twice as high as a healthier, more balanced meal. In healthy people, the pancreas takes care of this temporary elevation of blood sugar within an hour or two by parsing out extra doses of insulin. However, for people who are insulin resistant or have pre-diabetes or diabetes, repeated overproduction of insulin in response to large meals starts a vicious cycle that ultimately the pancreas can't keep up with. As a result, blood sugar builds up and stays up.
Getting Hungrier

Another cycle is created when you lose control of your blood sugar: hunger for more big meals. The first time you have an especially large meal, your insulin response can bring down your glucose levels so low that you want to eat more because your body thinks it's starving. This effect is exaggerated as you get older, according to a group of Tufts University researchers in the "Journal of Gerontology." In their experiment, older people who ate large meals of between 2,000 and 4,000 calories had more extreme blood sugar responses, and it took longer for their blood sugar to return to normal. Moreover, their poor blood sugar control impaired their ability to control their food intake.
Tips on Blood Sugar Levels

The Diabetes Action Research and Education Foundation advises you to make a habit of eating smaller, evenly spaced meals each day. The foundation also says that ideally, no one's blood sugar should go beyond 140 mg/dL, even after eating a large meal. Beyond that, you've entered a possible pre-diabetic diagnosis range. When it comes to holidays like Thanksgiving, the Joslin Diabetes Center recommends that you plan in advance, prepare desserts with sugar substitutes and stay within your recommended calorie range. If you have pre-diabetes, the National Diabetes Information Clearinghouse states that prevention of diabetes involves eating fewer calories to lose between 5 and 7 percent of your body weight.
- "Readers Digest": Why Blood Sugar Matters
- "Journal of Gerontology Series A"; Blood Glucose and Hormonal Responses to Small and Large Meals in Healthy Young and Older Women; K.J. Melanson et al.; July 1998
- Diabetes Action Research and Education Foundation: Blood Sugar Testing / Management
- "ABC News"; A Diabetic at the Thanksgiving Table; Katharine Gammon; Nov. 19, 2007
- Elmhurst College Virtual Chembook: Glucose; Charles Ophardt; 2003
- Joslin Diabetes Center: Tips for Making Truly Sweet Thanksgiving Desserts
- "Diabetes Forecast"; Remaking Thanksgiving Menus; Robyn Webb
- University of Illinois Extension: Your Guide to Diet and Diabetes
- MedlinePlus: Diabetes
- NDEP: Small Steps. Big Rewards. Your GAME PLAN to Prevent Type 2 Diabetes
Is this an emergency? If you are experiencing serious medical symptoms, please see the National Library of Medicine’s list of signs you need emergency medical attention or call 911.