
Often referred to as "chicken skin" or "goose bumps," keratosis pilaris is a common condition marked by tiny bumps on different parts of the skin. The bumps are usually painless and largely harmless, at least medically speaking.
The condition typically first appears in childhood and intensifies with the roiling hormones of puberty. It may completely disappear by the age of 30, although some cases persist well into adulthood. According to the Cleveland Clinic, some 50 to 80 percent of teenagers and 40 percent of adults will have keratosis pilaris at some point.
Video of the Day
Video of the Day
Many cases are mild and cause no problems. "It's really more of an annoyance," says board-certified dermatologist Roger I. Ceilley, MD, FAAD, clinical professor of dermatology at the University of Iowa Carver College of Medicine and past president of the American Academy of Dermatology (AAD).
For some folks, though, pronounced keratosis pilaris can lead to self-esteem issues.
There can also be stigma from a misperception that the condition results from poor hygiene, which is not the case, says Robert Anolik, MD, a New York City-based board-certified dermatologist and fellow of the American Academy of Dermatology.
Fortunately, keratosis pilaris often goes away permanently with time. Here's what else you need to know about this common skin condition.
Symptoms
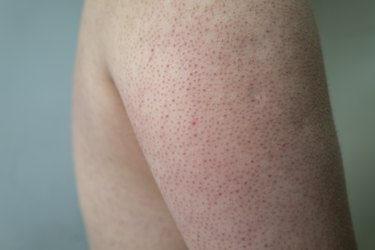
The defining symptom of keratosis pilaris are tiny bumps at the hair follicle, which most commonly appear on the upper arms, thighs and buttocks, although they can show up anywhere. These bumps — which some people describe as pimple-like — usually don't hurt or itch, according to the Mayo Clinic.
The bumps sometimes have tiny "horns" (thicker, rough skin) on top, Dr. Ceilley says. They may be concentrated together or scatttered in a given area.
The condition can affect people of any gender or race.
Here are other possible features:
- Dry, rough skin that feels like sandpaper
- The bumps can be the same color as your skin or they can be red, brown or white
- Areas with bumps can appear lighter or darker than the rest of your skin.
- Although sunlight has no effect on keratosis pilaris (good or bad), bumps from keratosis pilaris typically get worse in winter dryness and in dry climates
Although keratosis pilaris doesn't have any long-term consequences, aggressive scratching can cause scarring.
Causes
The rough, dry skin and other symptoms of keratosis pilaris happen when keratin — a protein in your hair, skin and nails — plugs up the hair follicles (pores) rather than molting off the skin as it should, explains Dr. Anolik. (Because the palms of your hands and soles of your feet don't have hair follicles, they aren't affected by keratosis pilaris.)
Sometimes the bumps have hairs tangled in them, but the condition can also lead to hair loss in the affected areas of the body.
As to what causes the keratin to build up, that's still an open question. "This isn't fully understood," says Dr. Anolik, although some think there are certain mutations that cause the disorder.
You may be at higher risk of developing keratosis pilaris if you:
- Have close family members with the condition
- Have asthma, eczema (atopic dermatitis) or hay fever
- Have dry skin
- Have overweight or obesity
- Have fair skin
- Have skin conditions like ichthyosis vulgaris
- Take the drug vemurafenib (Zelboraf) for melanoma (per the Mayo Clinic, this side effect tends to appear within two months of starting the drug and will disappear once the drug is stopped)
- Have diabetes, Down syndrome or hypothyroidism
According to the Cleveland Clinic, keratosis pilaris could be linked to vitamin A deficiency. It is not connected with gluten intolerance, although gluten intolerance can cause a skin rash that shares features with keratosis pilaris. A rash from gluten intolerance may look like a cluster of itchy, red bumps or blisters, and it commonly occurs on the knees, elbows, buttocks and hairline, per the Cleveland Clinic.
Diagnosis
Dermatologists and family physicians can typically diagnose keratosis pilaris just by looking at your skin. In fact, it's sometimes diagnosed when a doctor is examining you for a different reason, per the Mayo Clinic.
"It's a clinical appearance that's pretty classical," says Dr. Ceilley. "We wouldn't usually need a biopsy," or tissue sample.
Doctors may sometimes use a handheld device called a dermatoscope to get a closer look at the skin and hair follicles and confirm a diagnosis.
Medical Treatment
Most of the time, the condition can be taken care of at home. Keratosis pilaris medications like treatment creams Retin A or Retinol may be prescribed for more severe cases, says Dr. Ceilley. These prevent the hair follicles from getting blocked.
If medications don't work, providers sometimes turn to light treatment, laser therapy or microdermabrasion. Laser-assisted hair removal can get rid of ingrown hairs which may be contributing to the problem.
At-Home Remedies

Keratosis pilaris treatment at home usually includes a regular regimen of gentle exfoliation and moisturizing. Most plans take a few weeks to take effect. And, says Dr. Anolik, no matter which remedy you choose, "ongoing therapy is needed to maintain the benefits."
1. Use a Mild Cleanser
Use a mild, moisturizing body wash when you bathe to hydrate your skin and avoid irritating it.
Good options include:
- Cetaphil Ultra Gentle Body Wash ($7.97, Walmart.com)
- CeraVe Hydrating Body Wash ($11.99, Amazon)
- Purpose Gentle Cleansing Wash ($7.98, Walmart.com)
2. Remove Dead Skin Cells
To remove dead skin cells (exfoliate), use a cream or lotion designed to slough off dead skin (called a keratolytic) once a day.
In particular, look for creams and other products that contain alpha-hydroxy acid (AHA), glycolic acid, lactic acid, salicylic acid, urea or a retinoid (derived from vitamin A). These are available both over-the-counter and by prescription.
Many keratolytics also contain moisturizers to help with dry skin and itching that can accompany keratosis pilaris. Here are a few options:
You can also use a loofah or washcloth to exfoliate. "You have to be gentle," warns Dr. Ceilley. "Don't scrub or try to exfoliate these areas like you would with a brush or pumice, or you'll aggravate it."
3. Try Natural Exfoliants
There are home-remedy exfoliants that work for some people, but they have to be used carefully. The Cleveland Clinic has these suggestions:
- Apple cider vinegar contains AHA, but it can increase dryness and irritation. Dilute it with an equal amount of water and apply small amounts with a Q-tip.
- Baking soda mixed with warm water makes a paste that you can rub onto your skin in small, circular motions for about five minutes.
- Coconut oil can moisturize and may reduce discoloration and swelling.
4. Moisturize Often
Dry skin, which happens more often in winter months, can make the bumps more pronounced, per the AAD. To keep skin hydrated, apply a moisturizer after any keratolytic as well as after bathing (while you're still damp) and throughout the day.
Here are some other tips:
- Look for thicker creams such as Eucerin Original Healing Cream ($24.38, Amazon) or Cetaphil Moisturizing Cream ($15.97, Amazon).
- Fragrance is a common irritant. Stick to unscented products (this goes for soap as well) to avoid irritating and drying out the skin.
- Oil-free products will also preserve moisture.
5. Try Corticosteroids
A topical corticosteroid such as Cortizone 10 Maximum Strength Creme With Aloe ($4.86, Amazon) applied to the rough patches twice a day for one or two weeks can ease itching and redness. These are available both over-the-counter and by prescription.
6. Heed These Other Skin-Care Tips
"Avoiding certain bathing habits that dry the skin are fundamental to improving the appearance of keratosis pilaris," says Dr. Anolik. This includes:
- Limiting showers and baths to no more than 10 minutes
- Bathing in lukewarm or warm rather than very hot water
Here are other suggestions to incorporate throughout the day:
- Use a humidifier to keep the air moist
- Avoid wool and other itchy fabric as well as tight clothing, which can worsen bumps by rubbing, says Dr. Ceilley.
- Consider laser hair removal rather than shaving or waxing, which can also aggravate bumps
- Don't pick or scratch at the bumps, as this could lead to an infection
- Drink a lot of water
The Bottom Line
Although you can't cure or prevent keratosis pilaris, you can minimize any discomfort and improve the appearance of your skin with simple self-care strategies.
If this doesn't work after about six weeks or if the symptoms are severe, contact your primary care doctor or a dermatologist to see if more can be done.
- Mayo Clinic: “Keratosis Pilaris Symptoms and Causes”
- uptodate.com: “Keratosis pilaris”
- American Academy of Dermatology: “Keratosis Pilaris Overview”
- Robert Anolik MD, board certified dermatologist and Fellow of the American Academy of Dermatology
- U.K. National Health System: “Keratosis pilaris”
- DermNet NZ: “Keratosis pilaris”
- National Library of Medicine: “Keratosis pilaris”
- Medscape: “Keratosis Pilaris”
- Nationwide Children’s Hospital: “Keratosis Pilaris”
- American Academy of Family Physicians: “Keratosis Pilaris”
- Johns Hopkins Medicine: “Keratosis Pilaris”
- American Academy of Dermatology: “Keratosis Pilaris: Who Gets and Causes”
- Cleveland Clinic: “Keratosis Pilaris”
- American Academy of Dermatology: “Keratosis Pilaris: Signs and Symptoms”
- Mayo Clinic: “Keratin plug”
- Mayo Clinic: “Keratosis Pilaris Diagnosis and Treatment”
- American Academy of Dermatology: “Keratosis Pilaris Diagnosis and Treatment”
- Cleveland Clinic: "Dermatitis Herpetiformis"
Is this an emergency? If you are experiencing serious medical symptoms, please see the National Library of Medicine’s list of signs you need emergency medical attention or call 911.