Eczema and hives are easily confused because both have the same primary symptom: a ferocious rash on your skin.
But despite some similarities, these are two different conditions:
Video of the Day
Video of the Day
- Hives (referred to by doctors as urticaria) are bumps or raised patches on the skin, per the American Academy of Dermatology Association (AAD). Many things can trigger hives, such as an allergic reaction, but they're typically short-lived.
- Eczema is characterized by dry, itchy skin, and it's often long-lasting, according to the U.S. National Library of Medicine (NLM).
Neither of these uncomfortable conditions is contagious.
Here, discover the best ways to distinguish between these two skin conditions, along with dermatologists' tips for preventing and treating both hives and eczema, and learn when it's time for a doctor's visit.
Symptoms and Appearance
Hives Symptoms
- Itchy skin
- Swollen bumps
- Usually short-term
Eczema Symptoms
- Itchy skin
- Dry, rough or cracked skin
- Oozing
- Swelling
- Sometimes causes scaly patches
- Usually long-term
Itchiness is a uniting symptom for both hives and eczema.
But they're not wholly similar, which means there are ways to distinguish between them.
Hives

"Urticaria is characterized by transient skin swelling," says Natalie Hone, MD, a dermatologist at Memorial Hermann in Houston.
With hives, you'll have swollen bumps on your skin that may be flesh-colored or have a pink or red hue, Dr. Hone says. If you have black or brown skin, hives are likely to be a shade lighter or darker than your skin color, or the same color as your skin, and not red or pink, per the AAD.
They often look similar to bug bites, although sometimes they can be much larger and look like raised, well-defined welts.
"Usually, when you press on the affected area with a finger, the pink or red discoloration will disappear," Dr. Hone notes.
Hives are itchy, as mentioned before, and their size can vary from a few inches to the width and height of a hand. You may have a few hives or many, Dr. Hone says, and they can appear anywhere on your body.
"The key characteristic of hives is that individual lesions come and go rapidly, in general within 24 hours," Dr. Hone says.
Eczema
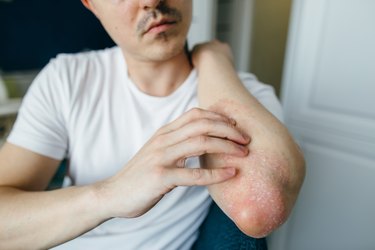
Eczema also changes the appearance of the skin.
"It can look like patches of skin that are swollen, pink to red, with fluid-filled bumps or thick, scaly plaques," Dr. Hone says.
Eczema can appear like hives, says board-certified internal medicine physician Chantel Strahan, MD. "However, eczema typically differs from hives because with eczema, the skin is typically very dry and rough, and you can have scaling of the skin," she says.
Other common symptoms of eczema are swelling, oozing skin, inflamed skin and scaly patches on your skin, per the National Eczema Association.
Causes
Hives Causes
- An allergic reaction
- Stress
- Unknown factors
Eczema Causes
- Allergic exposure (for contact dermatitis)
- Genetic and environmental factors (for atopic dermatitis)
Both hives and eczema can be triggered by an allergic reaction, but other causes are different.
Hives
Hives are often the result of an allergic reaction — to foods, medications or allergens. Something like a new laundry detergent or heat can trigger hives, per the Cleveland Clinic.
This allergic reaction triggers the release of histamine from immune cells found in your skin, Dr. Hone says. While your body intends for histamine to exert a protective force, it "causes that area of the skin to become raised, itchy, red and swollen," Dr. Hone says.
Stress is another factor that can lead to hives, according to the Cleveland Clinic. Viruses, too — even the common cold — are another common cause, according to Seattle Children's Hospital.
And sometimes the cause isn't clear: "Many cases are unexplained," Dr. Hone says.
Eczema
Eczema can also be the result of allergen exposures, Dr. Strahan says. That's known as contact dermatitis, and can be the result of a near-endless number of situations, including washing your hands frequently, touching something with fragrance or even contact with lemon juice followed by sunshine falling on your skin, per the AAD.
The more common form of eczema is atopic dermatitis. One in 10 people in the U.S. has this condition, according to the AAD. It often begins in childhood, Dr. Hone notes.
"It's a complex genetic disease with environmental influences," Dr. Hone says — that is, atopic dermatitis often runs in families. "It is known that there is a dysfunction of the skin barrier that can then cause environmental factors to sensitize and trigger inflammation," Dr. Hone notes, adding that it's associated with asthma, allergic rhinoconjunctivitis and other atopic conditions.
While eczema does not "spread," during flare-ups, more skin can be involved, Dr. Hone says.
Treatment
Hives Treatments
- Avoid triggers
- Steroids
- Immunotherapy (for chronic hives)
Eczema Treatments
- Avoid triggers
- Baby your skin
- Use topical medications
- Light therapy
- Injectable or oral medications
Hives
When it comes to hives, treatment is straightforward: Take an antihistamine. Stick to a non-drowsy med like Zyrtec ($14.80, Amazon) or Claritin ($25.12, Amazon) during the day. If you're taking it at night, Benadryl ($5.19, Amazon) is OK too.
This typically controls symptoms, Dr. Strahan says. Antihistamines can be topical or oral, depending on how much skin is involved, she says. For smaller areas, you can try an antihistamine cream like Benadryl Original Strength Cream ($6.78, Walmart.com).
To ease the itch, you can also use cooling lotions like calamine lotion ($7.70, Amazon) or those made with menthol, like Sarna ($10.12, Amazon), Dr. Hone says. (Consider these derm-recommended anti-itch creams, too.)
"Cold compresses also help to provide relief, especially for stress hives," Dr. Strahan says.
If hives don't respond to antihistamines, your doctor may recommend short-term use of systemic steroids, Dr. Hone says. Immunotherapy may be called for if you have chronic urticaria.
Eczema
Hives can be chronic but are not always. Eczema, on the other hand, is a chronic, incurable condition. That means it's important to maintain and improve the skin barrier through gentle skin care, Dr. Hone says.
Natural remedies for eczema include keeping showers short, applying moisturizers with glycerin and ceramides and/or creams with colloidal oatmeal, and taking baking-soda or bleach baths. You can also try coconut or sunflower oil on your skin.
It's also helpful to identify and avoid your triggers, such as stress, perfume or wool clothing, per the AAD.
And when flares occur, they're treated with topical medications (such as steroids) or with oral pills or injectables as needed, Dr. Hone says. More recent medications that treat the entire body include JAK inhibitors and biologics, and there are also older medications used which will suppress your immune system, per the AAD.
Light therapy can also be helpful; this is typically done either at the dermatologist's office or a phototherapy treatment center, according to the AAD.
Antihistamines can help ease the itch, per the Mayo Clinic — just make sure to take Benadryl and any other option that causes drowsiness at nighttime to avoid sleepiness during the day.
Prevention
Preventing Hives
- Avoid allergens and other triggers
Preventing Eczema
- Avoid triggers
- Be gentle with your skin
Hives
For hives, one of the best preventative tactics is to avoid your exposure to potential allergens. "Try switching to sensitive soaps and body lotions," Dr. Strahan says.
You can also try keeping a diary to see if you notice any links between hives and certain foods, activities or products.
But keep in mind that it depends on the type of hives: acute (lasting fewer than six weeks) or chronic (lasting more than six weeks), Dr. Hone says.
"A thorough evaluation and testing by a physician is key to determining the potential cause and avoidance," she adds.
That is, you'll need to try different tactics for avoiding hives if they spring up due to stress than if it's due to an ingredient frequently found in soap.
Eczema
When it comes to eczema, "maintaining a healthy skin barrier is key to avoid flares," Dr. Hone says. Here are her recommendations to do that:
- Take short showers and baths — and avoid hot water
- Use gentle soaps
- Moisturize daily
- Avoid your specific triggers
In general, you want to avoid having your skin get dry, Dr. Strahan says. While this may not be possible depending on where you live, try to also avoid cold and dry air, she says.
Other lifestyle changes for eczema management include managing stress, wearing loose clothing and assessing your diet, per the Cleveland Clinic.
When to See a Doctor
If your skin changes, it's likely time to see a doctor. That can help you determine exactly what's happening, and "establish a good treatment plan early," Dr. Hone says.
The doctor will do a clinical exam, take a history and perhaps do some tests to make a diagnosis, Dr. Hone says. "For example, patch testing is a test to diagnose contact dermatitis, which is an allergy to something your skin comes in contact with," she says.
The bottom line: Knowing early on if you have hives or eczema can help you avoid complications as well as appropriately treat the symptoms.
Warning
If you have hives along with tongue swelling, trouble breathing or speaking, gastrointestinal symptoms or a fever, seek medical care immediately.
- American Academy of Dermatology Association: "HIVES: OVERVIEW"
- U.S. National Library of Medicine: "Eczema"
- National Eczema Association: "What Is Eczema?"
- Cleveland Clinic: "Why Am I Breaking Out in Hives When I’m Stressed?!"
- AAD: "ECZEMA TYPES: CONTACT DERMATITIS OVERVIEW"
- AAD: "ECZEMA TYPES: ATOPIC DERMATITIS OVERVIEW"
- Mayo Clinic: "Atopic dermatitis (eczema)"
- Cleveland Clinic: "Here’s What’s Causing Your Eczema Flare-Up (and How To Prevent It)"
- Seattle Children's Hospital: "Hives"
Is this an emergency? If you are experiencing serious medical symptoms, please see the National Library of Medicine’s list of signs you need emergency medical attention or call 911.