With cold and flu season in full swing, and COVID-19 continuing to circulate, a lot of us are focused on how to stay healthy. From slurping up soup to bathing in hand sanitizer, you've probably read about a million different ways to avoid getting sick. But which prevention strategies actually work?
Below, medical experts separate fact from fiction to help set straight some of the most common germ myths.
Video of the Day
Video of the Day
1. Myth: Vitamin C Can Cure a Cold
When you're under the weather, you might reach for a tall glass of orange juice. But does a little vitamin C do the trick when you're sick?
"Vitamin C is important for immune defense, and we need a good immune function for healing," Pauline Jose, MD, a clinical instructor at UCLA and family medicine specialist at pH Labs, a national nonprofit health information organization, tells LIVESTRONG.com. That said, research has found that taking daily vitamin C supplements only modestly reduces a cold's duration, by about 8 percent, per the National Institutes of Health (NIH).
Vitamin C's ability to slightly shorten the length of a cold (and reduce the severity of your symptoms) may be in part because "it compensates for the increased inflammatory response and metabolic demand," Dr. Jose explains.
But if you just start popping vitamin C once you're already sick, it won't do much to speed your recovery, per the NIH.
At the end of the day, "the best remedy is good old-fashioned sleep," says Denise Pate, MD, board-certified internal medicine physician at Medical Offices of Manhattan. The more your body rests, the speedier your recovery. (Follow these strategies to get better sleep when you're sick.)
2. Myth: The Flu Is the Same as Having a Bad Cold
Though you may experience typical cold symptoms like sore throat, runny nose, sneezing, hoarseness and cough, the flu can be more dangerous than your run-of-the-mill common cold. The distinction is clear when you examine flu stats: Between 2010 and 2020, the flu led to 140,000 to 710,000 hospitalizations and 12,000 to 52,000 deaths annually, according to the Centers for Disease Control and Prevention (CDC).
And certain populations are at greater risk, including infants, the elderly, pregnant women and people with compromised immune systems, per the CDC. What's more, if you have a medical condition, such as heart disease, cancer or diabetes, the flu can lead to more serious complications.
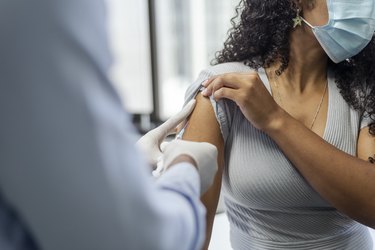
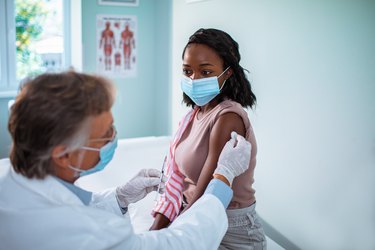
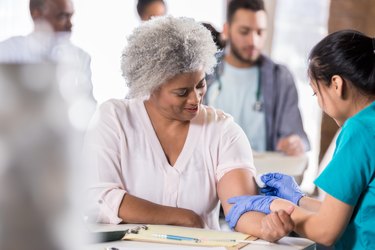
For this reason, Dr. Pate encourages people to get their annual flu vaccine. "Even if the shot doesn't prevent you from getting the flu, it can decrease the chance of developing severe symptoms," she says.
3. Myth: Healthy People Don't Need the Flu Vaccine

As mentioned above, certain groups have a higher risk for encountering flu-related complications, but "anyone is susceptible to contracting the flu, including healthy people," says Dr. Pate, adding that once infected, individuals can become contagious and spread the virus to others. That's why the CDC recommends that nearly everyone over 6 months of age, with rare exceptions, get vaccinated every flu season.
And getting the flu shot every year is key. "The influenza virus mutates, so getting vaccinated each year is important to make sure you have immunity to the strains most likely to cause an outbreak," Dr. Pate says.
4. Myth: You Need Antibiotics for the Flu
"False, false and false," Dr. Pate says about this belief. Antibiotics are specifically made to kill bacteria, not viruses like the flu or the novel coronavirus, which are completely different organisms.
"Supportive therapy, antiviral medications (not all viruses have medications) and preventative vaccines are the proper approach for treating viruses," she says. Taking Tamiflu, for instance, can potentially help reduce how long you're sick with the flu, per the CDC. But you need to take this antiviral within two days of getting sick, and it can cause unpleasant side effects (including stomach pains, fatigue and vomiting), according to the Food and Drug Administration. An antiviral medication is also available for COVID-19, per the CDC.
However, "sometimes a patient's immune function gets so challenged during a viral infection that they develop a superimposed bacterial infection like pneumonia," Dr. Jose says. In these cases, taking an antibiotic may be beneficial.
5. Myth: You Should 'Starve' a Fever

Feed a fever, starve a cold may be a common phrase — but it's also a total fiction. Though eating may be the last thing on your mind when you're under the weather, forgoing food may not be your best bet for a speedy healing process, Dr. Jose says.
Whether it's the cold or flu, "your immune system needs nutrients and energy to do its job, so eating and getting enough fluids is essential," Dr. Pate says.
Hydration is key for recovery. So if you can't choke down solids, try sipping on water, tea and broth.
6. Myth: The Flu Vaccine Causes the Flu
If you've ever gotten hit with the flu soon after receiving the flu shot, you might've assumed that the vaccine itself made you ill. But this simply isn't true. "The flu shot is made from an inactivated virus that can't transmit infection," Dr. Pate says.
In fact, it takes a week or two for the vaccine's protection to kick in, so people who become symptomatic immediately after getting a flu shot were already on their way to getting sick before they got vaccinated, Dr. Pate explains.
7. Myth: Wearing Gloves Can Prevent You From Picking Up Germs

Hate to break it to you, but wearing gloves — whether winter gloves or the surgical kind — isn't the best way to avoid germs.
Gloves are like a second skin. That is, they pick up the same pathogens your bare hands do. Subsequently, they can also transmit — and infect you with — harmful bugs if you touch an unclean surface and then touch your face, according to Flushing Hospital Medical Center.
In other words, for gloves to serve any protective function at all, you would have to wash (or change) them as regularly as you would your ungloved hands — which pretty much defeats the purpose of wearing them.
However, if you're caring for someone with an illness like COVID-19, the CDC recommends you don disposable gloves when coming into contact with the person's blood, stool or body fluids (including saliva, sputum, nasal mucus, vomit and urine). This also goes for when you clean "high-touch" surfaces, such as counters, tabletops, doorknobs, bathroom fixtures, toilets, phones and keyboards, and when handling soiled clothing and bedding for laundry.
In these cases, always avoid touching your eyes, nose and mouth with gloved hands. Then dispose of them immediately (only use them once!) and wash your hands straightaway with soap and water for at least 20 seconds, per the CDC.
- Centers for Disease Control and Prevention: “Who Should and Who Should NOT Get a Flu Vaccine”
- JAMA: “Medical Masks.”
- Flushing Hospital Medical Center: “How Can Wearing Gloves Get You Sick?”
- National Institutes of Health: “Vitamin C: Fact Sheet for Health Professionals.”
- Centers for Disease Control and Prevention: "Use of Cloth Face Coverings to Help Slow the Spread of COVID-19"
- CDC: "Treatment: What You Need to Know"
- Food and Drug Administration: "Tamiflu: Consumer Questions and Answers"
- CDC: "COVID-19 Treatments and Medications"
- CDC: "Caring for Someone Sick at Home"
- CDC: "Inactivated Influenza VIS"
- Centers for Disease Control and Prevention: "Disease Burden of the Flu"
Is this an emergency? If you are experiencing serious medical symptoms, please see the National Library of Medicine’s list of signs you need emergency medical attention or call 911.