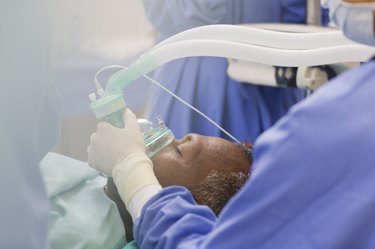
You might have heard that the prep for a colonoscopy is worse than the procedure itself. That may be true: You're sedated for the actual colonoscopy, which involves a gastroenterologist inserting a colonoscope — a long, thin tube with a camera on one end — into your colon (definitely not something you want to be aware of).
Sedation allows you to be relaxed and even asleep while the colonoscopy is happening. Many people don't even remember what happened during the procedure.
Video of the Day
Video of the Day
Types of Colonoscopy Sedation
There are two basic forms of sedation for a colonoscopy procedure: conscious sedation and anesthesia.
"Conscious sedation is when the physician [conducting the colonoscopy] directs the administration of the sedation," says John H. Ashcraft, DO, chief of colon and rectal surgery at the University of Kansas Health System in Kansas City. In other words, during conscious sedation, the doctor doing the procedure oversees both the colonoscopy and the sedation. Conscious sedation involves cardiac monitoring and light oxygen therapy. A nurse is responsible for administering the sedation through an IV while the physician performs the procedure.
Read more: Can I Eat Colored Jell-O Before a Colonoscopy?
Conscious sedation is typically a lighter level of sedation, and patients usually can be awakened at any time. In reality, however, responses to different sedatives vary greatly among patients, according to Yale Medicine. Drugs used for conscious sedation include midazolam (Versed) and fentanyl.
Anesthesia drugs, on the other hand, produce a deeper sedation and have to be administered by an anesthesiologist or a nurse anesthetist while the gastroenterologist performs the colonoscopy. Two doctors (rather than a doctor and a nurse, as during conscious sedation) are present because of the higher sedation and the associated risks (like low blood pressure or slowed breathing), for which they can give other drugs or more aggressive oxygen therapy, according to Temple Health.
Different colonoscopy facilities have different preferences when it comes to sedation. Dr. Ashcraft prefers to use anesthesia, because it leaves him free to focus on the actual colonoscopy. "I have all my attention there," he says.
Here are the three main drugs used to sedate colonoscopy patients. Often, doctors use more than one.
Midazolam
According to an analysis of 1.4 million colonoscopies published in May 2016 in Gastroenterology & Hepatology, midazolam, also known as Versed, is the most common drug used for colonoscopies. It induces a state of conscious sedation and is a benzodiazepine, a class of medication which also includes Xanax. Midazolam slows brain activity, so after being sedated with it, you most likely won't remember the procedure. Midazolam is often used in combination with the narcotic drug fentanyl.
Fentanyl
This is the most common narcotic (opioid) used for colonoscopy procedures. You've likely heard about it in relation to the opioid crisis engulfing the U.S. According to Harvard Health Publishing, fentanyl is more powerful than oxycontin, morphine or heroin. In the confines of a relatively quick colonoscopy, though, it doesn't pose any addiction or dependency danger, according to Dr. Ashcraft. "There's minimal risk," he says. "There aren't any issues for such a brief, temporary procedure."
Propofol
Nicknamed the "milk of anesthesia" (mainly because of its white color), propofol — aka Diprivan — is an anesthetic and must be administered by an anesthesiologist. According to Yale Medicine, it acts quickly, knocking you out in around five minutes. It wears off quickly, too: Most patients are awake again within 15 minutes of its final administration.
Read more: How to Recover After a Colonoscopy
Less Common Colonoscopy Sedatives
A few other medications are also used for colonoscopies. One is meperidine (Demerol). It's a narcotic and is used to induce conscious sedation. Per the Cleveland Clinic, diazepam — aka Valium — is sometimes used instead of midazolam.
The drug diphenhydramine — which is actually the antihistamine Benadryl — is sometimes used for patients who have trouble being sedated, perhaps because they've been on long-term opioid therapy, according to a May 2018 article in Gastrointestinal Endoscopy. Diphenhydramine can also be used for patients who are particularly anxious before the procedure, and it can be combined with fentanyl and midazolam, according to the Gastroenterology & Hepatology analysis.
Sedative Side Effects
Each of these drugs has its own side-effect profile, but one thing all sedatives have in common is that they slow down breathing, occasionally to a dangerous degree. That is why colonoscopy patients have to be monitored so closely.
While sedation will help you feel comfortable during the colonoscopy procedure, it will also make you feel tired and groggy for up to 24 hours after the procedure, which is why you will need someone to help you get home from the appointment, according to the Cleveland Clinic.
Talk to your doctor about the different sedative options prior to your colonoscopy, so the two of you can determine which sedative would be most appropriate for you.
- Gastroenterology & Hepatology: “Sedation in Colonoscopy”
- Gastrointestinal Endoscopy: “Practice Patterns of Sedation for Colonoscopy”
- Yale Medicine: “Anesthesia for Colonoscopy”
- Cleveland Clinic: “Colonoscopy Procedure: Colonoscopy Instructions”
- National Library of Medicine: “Midazolam Injection”
- Temple Health: “What Are My Options for Sedation During My Upcoming Colonoscopy?”
- Harvard Medical School: “Fentanyl: The Dangers of This Potent ‘Man-Made’ Opioid”
- National Library of Medicine: “Meperidine”
- Gastrointestinal Endoscopy: “Use of Diphenhydramine as an Adjunctive Sedative for Colonoscopy in Patients on Chronic Opioid Therapy: A Randomized Controlled Trial”
- American Society for Gastrointestinal Endoscopy: “Guidelines for Sedation and Anesthesia in GI Endoscopy”
Is this an emergency? If you are experiencing serious medical symptoms, please see the National Library of Medicine’s list of signs you need emergency medical attention or call 911.